Removal of the sac during surgery for the repair of "giant" paraesophageal hernias
- PMID: 40740916
- PMCID: PMC12305281
- DOI: 10.4240/wjgs.v17.i7.106365
Removal of the sac during surgery for the repair of "giant" paraesophageal hernias
Abstract
Background: The presence of a large paraesophageal hernia is a source of concern in foregut surgery. Thus, scholars have focused on ascertaining the optimal surgical approach, methods for reinforcing the esophageal hiatus, and strategies for preventing hernia recurrence and gastroesophageal reflux.
Aim: To investigate the outcomes of surgery for giant paraesophageal hernias without sac removal.
Methods: Sixty-six consecutive patients who underwent surgery for a giant paraesophageal hernia between May 2010 and December 2024 were included in this retrospective study. The pre- and postoperative examinations included upper gastrointestinal endoscopy, X-ray with barium contrast swallow, contrast-enhanced computed tomography (CT) scans of the chest and abdomen, 24-hour potential hydrogen esophageal monitoring, and esophagomanometry. The study group included 36 patients who underwent surgery without sac removal, and the control group included 30 patients who underwent surgery with sac removal.
Results: Fifty-two patients (28 in the study group and 24 in the control group) underwent laparoscopic procedures, 10 (6 in the study group and 4 in the control group) underwent open procedures, and 4 (2 in each group) underwent conversion procedures. The operative time and postoperative length of stay were significantly longer in the control group than in the study group. In 12 patients in the study group, X-ray examination on postoperative days 3-5 revealed air-fluid levels at the site of the remaining hernia sac; all air-fluid levels disappeared without intervention 2 months later. Postoperative day 60 CT and X-ray examinations revealed no pathological changes related to the hernia sac in the mediastinum.
Conclusion: Removal of the hernia sac during surgery for giant paraesophageal hernias is not mandatory. Further large-scale multicentric randomized trials are needed for a more detailed investigation in this field.
Keywords: Hernia repair; Hernia sac; Hiatal hernia; Laparoscopic fundoplication; Paraesophageal hernia.
©The Author(s) 2025. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: The authors declare that they have no conflicts of interest.
Figures
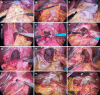
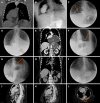
Similar articles
-
Restoration of normal anatomy without fundoplication in non-elective incarcerated giant paraesophageal hernia repair.Surg Endosc. 2025 Jul 14. doi: 10.1007/s00464-025-11924-w. Online ahead of print. Surg Endosc. 2025. PMID: 40659950
-
Transabdominal pre-peritoneal (TAPP) versus totally extraperitoneal (TEP) laparoscopic techniques for inguinal hernia repair.Cochrane Database Syst Rev. 2024 Jul 4;7(7):CD004703. doi: 10.1002/14651858.CD004703.pub3. Cochrane Database Syst Rev. 2024. PMID: 38963034 Free PMC article.
-
Mesh versus non-mesh for inguinal and femoral hernia repair.Cochrane Database Syst Rev. 2018 Sep 13;9(9):CD011517. doi: 10.1002/14651858.CD011517.pub2. Cochrane Database Syst Rev. 2018. PMID: 30209805 Free PMC article.
-
Recovery after abdominal wall reconstruction.Dan Med J. 2017 Mar;64(3):B5349. Dan Med J. 2017. PMID: 28260602
-
Laparoscopic techniques versus open techniques for inguinal hernia repair.Cochrane Database Syst Rev. 2003;2003(1):CD001785. doi: 10.1002/14651858.CD001785. Cochrane Database Syst Rev. 2003. PMID: 12535413 Free PMC article.
References
-
- Kohn GP, Price RR, DeMeester SR, Zehetner J, Muensterer OJ, Awad Z, Mittal SK, Richardson WS, Stefanidis D, Fanelli RD SAGES Guidelines Committee. Guidelines for the management of hiatal hernia. Surg Endosc. 2013;27:4409–4428. - PubMed
-
- Ténaiová J, Tůma L, Hrubant K, Brůha R, Svestka T, Novotný A, Petrtýl J, Jirásek V, Urbánek P, Lukás K. [Incidence of hiatal hernias in the current endoscopic praxis] Cas Lek Cesk. 2007;146:74–76. - PubMed
-
- Landreneau RJ, Del Pino M, Santos R. Management of paraesophageal hernias. Surg Clin North Am. 2005;85:411–432. - PubMed
-
- Skinner DB, Belsey RH. Surgical management of esophageal reflux and hiatus hernia. Long-term results with 1,030 patients. J Thorac Cardiovasc Surg. 1967;53:33–54. - PubMed
LinkOut - more resources
Full Text Sources

