Triple reversal phenomenon in EGFR-mutant lung adenocarcinoma with prostate metastasis following hepatocellular carcinoma: a rare Case Report with diagnostic and therapeutic implications
- PMID: 40740944
- PMCID: PMC12307205
- DOI: 10.3389/fmed.2025.1619466
Triple reversal phenomenon in EGFR-mutant lung adenocarcinoma with prostate metastasis following hepatocellular carcinoma: a rare Case Report with diagnostic and therapeutic implications
Abstract
Background: Non-small cell lung cancer harboring EGFR mutations is responsive to targeted therapies such as Osimertinib. Although metastasis from lung cancer to the prostate is exceedingly rare, we present a rare case of prostatic metastasis from lung adenocarcinoma in a patient with a history of hepatocellular carcinoma (HCC) and no evidence of a primary lung lesion.
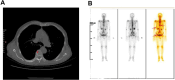
Case presentation: A 64-years-old male with chronic hepatitis B and a history of hepatocellular carcinoma (HCC) diagnosed in 2014 presented in 2023 with elevated carcinoembryonic antigen (CEA) levels. Initial imaging revealed isolated bone metastasis, initially presumed to be recurrent HCC. Given the long interval since diagnosis, a bone biopsy was performed, unexpectedly showing adenocarcinoma. Subsequent PET-CT identified a prostatic lesion without pulmonary abnormalities, leading to an initial diagnosis of metastatic prostate cancer. Prostate biopsy, however, revealed features consistent with lung adenocarcinoma. Molecular testing detected an EGFR exon 21 L858R mutation, confirming metastatic lung adenocarcinoma. The patient responded favorably to osimertinib therapy.
Conclusion: This case illustrates a rare instance of prostatic metastasis from EGFR-mutant lung adenocarcinoma and emphasizes the critical role of repeat biopsy, molecular profiling, and multidisciplinary evaluation in atypical metastatic presentations. The diagnostic process involved a "triple reversal" phenomenon, revising initial misdiagnoses of recurrent HCC and primary prostate cancer to metastatic NSCLC. Targeted therapy with osimertinib was effective, underscoring the importance of precision oncology in managing complex metastatic disease.
Keywords: EGFR mutation; case report; lung adenocarcinoma; multidisciplinary approach; prostate metastasis; targeted therapy; triple reversal phenomenon.
Copyright © 2025 Luo, Zhou and Liu.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures



References
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

