Renal cancer survival in clear cell renal cancer compared to other types of tumor histology: A population-based cohort study
- PMID: 40743229
- PMCID: PMC12312934
- DOI: 10.1371/journal.pone.0329000
Renal cancer survival in clear cell renal cancer compared to other types of tumor histology: A population-based cohort study
Erratum in
-
Correction: Renal cancer survival in clear cell renal cancer compared to other types of tumor histology: A population-based cohort study.PLoS One. 2026 Jan 29;21(1):e0342010. doi: 10.1371/journal.pone.0342010. eCollection 2026. PLoS One. 2026. PMID: 41610091 Free PMC article.
Abstract
Introduction: Renal cancer (RC) presents a challenge with increasing incidence and mortality. This study compares RC cancer-specific survival (CSS) and overall survival (OS) based on histological type.
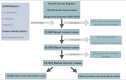
Study design: This population-based retrospective cohort study covers 1995-2017, utilizing cases from the Finnish Cancer Registry. Comorbidity, procedure and treatment information from 1995-2018 were obtained from the national health care registry, while death data originated from the national death certificate registry. RC cases were categorized by histology to analyze CSS and OS via Fine and Gray's proportional sub-hazards model and Cox regression (adjusting for age, tumor extent, Charlson comorbidity index and treatment).
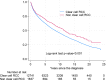
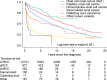
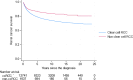
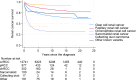
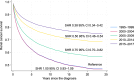
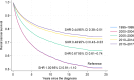
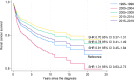
Results: The final cohort included 14,413 patients, predominantly ccRCC (75.5%), followed by papillary RCC (pRCC),5.8% and chromophobe RCC (chRCC) 2.1%. Univariate analysis showed better OS for non-ccRCC patients, with 5-year survival (5ySR) of 72.6% (95% CI 70.3-74.7%), compared to ccRCC (62.7%, 95%CI 61.8-63.5). Among non-ccRCC, the 5ySRs were as follows: pRCC 74.3% (95%CI 71.2-77.2), chRCC 82.2% (95% CI 77.2-86.1), sarcomatoid variants (sarcRC) 29.2% (95% CI 20.6-38.3), and collecting duct carcinoma (CDC) 23.5% (95%CI 7.3-44.9). Non-ccRCC showed improved CSS compared to ccRCC (sHR 0.69, 95% CI 0.60-0.78). Favorable CSS for chRCC (sHR 0.28, 95% CI 0.18-0.43) and pRCC (sHR 0.66, 95% CI 0.56-0.78), while sarcRC (sHR 1.83, 95% CI 1.36-2.46) and CDC (sHR 3.19, 95% CI 2.01-5.08) showed poorer CSS. Overall, non-ccRCC had a better prognosis, driven by pRCC and chRCC, whereas sarcRC and CDC had poor prognoses. CSS has improved over time, with a 62% reduction in death risk since 1995.
Conclusion: Our results demonstrate that the histological subtype is a powerful predictor of survival. Histology should be used more in clinical decision-making. Having a histological confirmation would tailor the selection of treatment: surgical management for aggressive and ccRCC and conservative management for less aggressive histological types.
Copyright: © 2025 Sepp et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
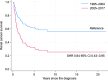
References
-
- European cancer information system. Europa.eu. Published October 19, 2017. [cited September 19, 2023]. Available from: https://ecis.jrc.ec.europa.eu/explorer.php?$0-0$1-AE28E$4-1,2$3-All$6-0,...
-
- Ferlay J, Ervik M, Lam F, Laversanne M, Colombet M, Mery L, et al. Global Cancer Observatory: Cancer Today. Lyon, France: International Agency for Research on Cancer. 2024. , [cited 12 September 2024]. Available from: https://gco.iarc.who.int/today
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

