Immediate efficacy of low-intensity focused ultrasound versus planar ultrasound in patients with myofascial pain syndrome of upper trapezius: a randomized controlled clinical trial
- PMID: 40745538
- PMCID: PMC12312598
- DOI: 10.1186/s12891-025-09017-9
Immediate efficacy of low-intensity focused ultrasound versus planar ultrasound in patients with myofascial pain syndrome of upper trapezius: a randomized controlled clinical trial
Abstract
Background: Myofascial pain syndrome (MPS), a chronic musculoskeletal disorder characterized by myofascial trigger points (MTrPs), causes localized pain and dysfunction. The objective is to compare the immediate therapeutic effects of low-intensity focused ultrasound (LIFU) versus low-intensity planar ultrasound (LIPU) on pain and function in upper trapezius MPS.
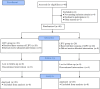
Method: This study was designed as a single-blind, randomized controlled trial. The patients (20 ≤ aged ≤ 70) diagnosed with MPS of the upper trapezius were randomly allocated to either LIFU (study group; n = 20; 9 men, 11 women) or LIPU (control group; n = 20; 15 men, 5 women) treatments (1.5 W/cm2, 1 MHz, 5 min, once a day, 3 days). The primary outcome was pain severity, assessed immediately post-treatment using the Visual Analog Scale (VAS; 0 ~ 10 cm), and served as the central efficacy endpoint. Secondary outcomes comprised supplemental assessments including: (1) multidimensional pain characterization via the Short-Form McGill Pain Questionnaire (SF-MPQ); (2) functional disability quantification through the Neck Disability Index (NDI); and (3) neuromuscular biomarkers measured by surface electromyography (sEMG) parameters (root mean square [RMS], median frequency [MF]). The outcomes were assessed before treatment and 10 min, 72 h after completing the third and final session of treatment.
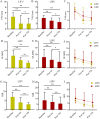
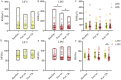
Results: Pain intensity, as measured by the VAS, decreased significantly immediately after treatment in both the LIFU group (median difference [MD] = -2.0 cm; 95% confidence interval [CI]: -2.5 to -1.5 cm; p = 0.002) and the LIPU group (MD = -1.0 cm; 95% CI: -1.5 to -0.5 cm; p = 0.001), with these reductions maintained at 72 h post-treatment. Both SF-MPQ and NDI scores showed significant improvements following treatment in both groups. A significant reduction in RMS parameters was observed in the LIPU group immediately after treatment (MD = -15.3 µV; 95% CI: -20.0 to -10.5 µV; p = 0.028). No significant differences were observed between the groups in terms of pain alleviation, functional improvement, and alterations in neuromuscular electrophysiological activity (p > 0.05); however, moderate to large effect sizes suggest possible clinical relevance. No adverse events were reported.
Conclusion: Both LIFU and LIPU can be considered effective therapeutic options, offering immediate symptom relief in patients with upper trapezius MPS.
Trial registration: The protocol was registered at the Chinese Clinical Trial Register (ChiCTR2500097431) as a clinical trial on 19/02/2025 http://www.chictr.org.cn/ .
Keywords: Low-intensity focused ultrasound; Low-intensity planar ultrasound; Myofascial pain syndrome; Myofascial trigger points; Surface electromyography; Upper trapezius.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: This study design was approved by the Ethics Committee for Biomedical Research of West China Hospital of Sichuan University (Approval number: 2023 − 251). All procedures performed in this study were in accordance with the ethical standards of the 1964 Helsinki Declaration. The consent was obtained from all of the participants prior to the study. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures
Similar articles
-
Prescription of Controlled Substances: Benefits and Risks.2025 Jul 6. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2025 Jul 6. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 30726003 Free Books & Documents.
-
Ultrasound-guided injection of platelet-rich plasma alleviated pain and improved function for individuals with myofascial pain syndrome: a retrospective case series study.BMC Musculoskelet Disord. 2025 Jul 4;26(1):648. doi: 10.1186/s12891-025-08884-6. BMC Musculoskelet Disord. 2025. PMID: 40616050 Free PMC article.
-
Efficacy of temporo-parietal fascia trigger point release in the management of tension-type headache: a single-blinded RCT.Pain Manag. 2025 Aug;15(8):509-517. doi: 10.1080/17581869.2025.2527616. Epub 2025 Jul 12. Pain Manag. 2025. PMID: 40650965 Clinical Trial.
-
Ultrasound and shockwave therapy for acute fractures in adults.Cochrane Database Syst Rev. 2014 Jun 23;2014(6):CD008579. doi: 10.1002/14651858.CD008579.pub3. Cochrane Database Syst Rev. 2014. Update in: Cochrane Database Syst Rev. 2023 Mar 3;3:CD008579. doi: 10.1002/14651858.CD008579.pub4. PMID: 24956457 Free PMC article. Updated.
-
Ultrasound and shockwave therapy for acute fractures in adults.Cochrane Database Syst Rev. 2023 Mar 3;3(3):CD008579. doi: 10.1002/14651858.CD008579.pub4. Cochrane Database Syst Rev. 2023. PMID: 36866917 Free PMC article.
References
-
- Simons DG, Travell JG. Myofascial origins of low back pain. 1. Principles of diagnosis and treatment. Postgrad Med. 1983;73(2):66, 68–70, 73 passim. 10.1080/00325481.1983.11697756. - PubMed
-
- Lam C, Francio VT, et al. Myofascial pain - a major player in musculoskeletal pain. Best Pract Res Clin Rheumatol. 2024;38(1): 101944. 10.1016/j.berh.2024.101944. - PubMed
-
- Urits I, Charipova K, et al. Treatment and management of myofascial pain syndrome. Best Pract Res Clin Anaesthesiol. 2020;34(3):427–48. 10.1016/j.bpa.2020.08.003. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

