Interstitial Nephritis Induced by Repeated Nonsteroidal Anti-inflammatory Drugs (NSAIDs) Use for Persistent Fever: A Case Report
- PMID: 40761978
- PMCID: PMC12319171
- DOI: 10.7759/cureus.87304
Interstitial Nephritis Induced by Repeated Nonsteroidal Anti-inflammatory Drugs (NSAIDs) Use for Persistent Fever: A Case Report
Abstract
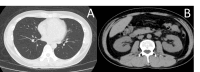
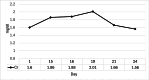
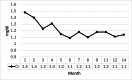
Nonsteroidal anti-inflammatory drugs (NSAIDs) are extensively utilized for their analgesic and anti-inflammatory efficacy, yet they pose a significant risk for renal adverse events, notably drug-induced acute interstitial nephritis (DI-AIN). Prompt recognition and appropriate management are paramount to prevent irreversible kidney damage. We present the case of a 46-year-old male with NSAID-induced DI-AIN, emphasizing the diagnostic utility of a specific urinary biomarker profile and the rationale for empirical steroid therapy initiated before histopathological confirmation. Our patient developed acute kidney injury (AKI) following daily ibuprofen administration for persistent fever. Despite ibuprofen discontinuation on day eight, renal function failed to improve, necessitating hospital admission on day 14. On day 15, his serum creatinine (Cr) level was 1.86 mg/dL. Urinalysis revealed mild proteinuria [urine protein-to-creatinine ratio (UPCR): 0.24 g/gCr] but strikingly elevated urinary tubular injury markers: N-acetyl-β-D-glucosaminidase (NAG): 20.9 U/L (on day one), β2-microglobulin (β2MG): 6028 μg/L, and L-type fatty acid-binding protein (L-FABP): 27.75 ng/mL. Based on a strong clinical suspicion of DI-AIN, a kidney biopsy was performed on day 15, and oral prednisolone (PSL, 0.8 mg/kg/day) was commenced the same evening before biopsy results were available. Serum creatinine improved to 1.56 mg/dL by discharge on day 23. Post-discharge, kidney biopsy results confirmed AIN. PSL was gradually tapered and discontinued after approximately 10 months, with sustained renal function recovery (serum creatinine: ~1.1 mg/dL). This report underscores the importance of suspecting DI-AIN in patients with AKI and a history of NSAID exposure. The pronounced elevation of urinary tubular markers, despite only mild proteinuria, was pivotal in raising clinical suspicion. The negative autoimmune serology further strengthened the diagnosis of a drug-induced etiology. Empirical steroid therapy, initiated due to compelling clinical evidence before histopathological confirmation, appeared to be an effective intervention. While this single case cannot establish a therapeutic standard, it illustrates a clinical scenario where early, empirically-guided treatment may be justified. Kidney biopsy remains indispensable for definitive diagnosis. The report also highlights the pressing need for enhanced patient education on appropriate NSAID utilization. Repeated use of common NSAIDs can precipitate DI-AIN. A diagnostic profile of elevated urinary tubular markers with only mild proteinuria can be a key indicator for suspecting this condition. Empirical steroid therapy, guided by strong clinical suspicion, can be an effective early intervention, with subsequent kidney biopsy providing definitive diagnostic validation. Enhanced patient education on appropriate NSAID use is essential.
Keywords: #aki; acute interstitial nephritis (ain); drug induced aki; n-acetyl glucosaminidase(nag); nsaid abuse; steroid use.
Copyright © 2025, Yoshida et al.
Conflict of interest statement
Human subjects: Informed consent for treatment and open access publication was obtained or waived by all participants in this study. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures

References
-
- Usage and prescribing patterns of NSAIDs in different general and specialized hospitals in Bangladesh. Gani D, Parveen P, Saha D, et al. Sch Acad J Pharm. 2022;11:161–166.
-
- Physician perspectives on non-steroidal anti-inflammatory drugs: a comprehensive survey on usage and preferences. Gondane A, Pawar D. Int J Basic Clin Pharmacol. 2024;13:696–701.
-
- Effects of nonsteroidal anti-inflammatory meloxicam on stomach, kidney, and liver of rats. Burukoglu D, Baycu C, Taplamacioglu F, Sahin E, Bektur E. Toxicol Ind Health. 2016;32:980–986. - PubMed
-
- A retrospective database study of gastrointestinal events and medical costs associated with nonsteroidal anti-inflammatory drugs in Japanese patients of working age with osteoarthritis and chronic low back pain. Kikuchi S, Togo K, Ebata N, Fujii K, Yonemoto N, Abraham L, Katsuno T. Pain Med. 2021;22:1029–1038. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
