Postnatal antibiotic exposure due to maternal group B streptococcus is associated with childhood asthma
- PMID: 40762188
- PMCID: PMC12322942
- DOI: 10.1111/pai.70167
Postnatal antibiotic exposure due to maternal group B streptococcus is associated with childhood asthma
Abstract
Background: Previous studies identified early-life antibiotic exposure as a risk factor for childhood asthma. However, this association may be confounded by an indication, as antibiotics are often prescribed for respiratory infections, which themselves promote asthma. To mitigate this bias, we aim to assess the unique contribution of postnatal antibiotic therapy, given to non-infected infants for maternal indication, on childhood asthma risk.
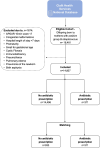
Methods: We screened electronic medical records to identify healthy full-term infants born during 2006-2018 to mothers with a positive group B streptococcus (GBS) vaginal culture. Infants with postnatal respiratory symptoms/pneumonia or positive blood/cerebrospinal fluid cultures were excluded. The primary outcome was an asthma diagnosis by age 6 years. We fitted a multivariable quasi-Poisson regression model to assess the unique contribution of antibiotic treatment to asthma diagnosis. As a validation step, we utilized a propensity model in which infants treated with antibiotics were matched 1:3 with infants not treated.
Results: The cohort included 14,807 infants, of whom 311 received antibiotics. After controlling for potential confounders, postnatal antibiotic exposure was associated with higher asthma risk (adjusted risk ratio [aRR] = 1.3, 95%; confidence interval [CI] 1.04-1.61, p = .017). Higher asthma risk was validated in the propensity model (aRR = 1.49, 95% CI 1.12-1.96 p = .005). Postnatal antibiotic therapy was also associated with secondary outcomes such as the short-acting beta-ag use (aRR = 1.13, 95% CI 0.99-1.28, p = .072) and allergic rhinitis diagnosis (aRR = 3.00, 95% CI 1.43-6.30, p = .003).
Conclusions: Postnatal antibiotic therapy administrated for maternal GBS, not confounded by infants' infections, was associated with higher childhood asthma risk.
Keywords: asthma; group B streptococcus; postnatal antibiotic exposure.
© 2025 The Author(s). Pediatric Allergy and Immunology published by European Academy of Allergy and Clinical Immunology and John Wiley & Sons Ltd.
Conflict of interest statement
The authors do not have any conflicts of interest related to this work.
Figures

Similar articles
-
Vaginal chlorhexidine during labour to prevent early-onset neonatal group B streptococcal infection.Cochrane Database Syst Rev. 2014 Dec 14;2014(12):CD003520. doi: 10.1002/14651858.CD003520.pub3. Cochrane Database Syst Rev. 2014. PMID: 25504106 Free PMC article.
-
Antibiotics for exacerbations of asthma.Cochrane Database Syst Rev. 2018 Jun 25;6(6):CD002741. doi: 10.1002/14651858.CD002741.pub2. Cochrane Database Syst Rev. 2018. PMID: 29938789 Free PMC article.
-
Interventions for managing asthma in pregnancy.Cochrane Database Syst Rev. 2014 Oct 21;2014(10):CD010660. doi: 10.1002/14651858.CD010660.pub2. Cochrane Database Syst Rev. 2014. PMID: 25331331 Free PMC article.
-
Antiretroviral therapy (ART) for treating HIV infection in ART-eligible pregnant women.Cochrane Database Syst Rev. 2010 Mar 17;2010(3):CD008440. doi: 10.1002/14651858.CD008440. Cochrane Database Syst Rev. 2010. PMID: 20238370 Free PMC article.
-
Interventions for treating genital Chlamydia trachomatis infection in pregnancy.Cochrane Database Syst Rev. 2017 Sep 22;9(9):CD010485. doi: 10.1002/14651858.CD010485.pub2. Cochrane Database Syst Rev. 2017. PMID: 28937705 Free PMC article.
References
-
- American Academy of Asthma Allergy &Immunology . AAAAI asthma statistics.
-
- Global Initiative for Asthma . Global strategy for asthma management and prevention. 2024.
-
- Beasley R, Semprini A, Mitchell EA. Risk factors for asthma: is prevention possible? Lancet. 2015;386(9998):1075‐1085. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

