Ghrelin improves small intestinal barrier damage in sepsis by promoting miR-143/ATG2B-mediated autophagy
- PMID: 40773487
- PMCID: PMC12331055
- DOI: 10.1371/journal.pone.0329488
Ghrelin improves small intestinal barrier damage in sepsis by promoting miR-143/ATG2B-mediated autophagy
Abstract
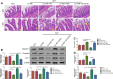
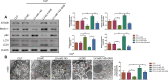
Intestinal barrier damage is crucial for the development of sepsis. Ghrelin (GHS) can restore intestinal barrier function. However, the mechanisms of GHS on intestinal barrier damage in sepsis remain unclear. We aimed to explore the mechanisms of GHS against intestinal barrier damage in sepsis. Septic models were established by cecal ligation and puncture surgery for rats and lipopolysaccharides exposure for IEC-6 cells. Furthermore, these septic models were overexpressed miR-143 and treated with GHS. In vivo, small intestinal pathological injury and D-lactic acid level were detected. Tight junction protein (Claudin-1, Occludin and ZO-1) expressions and autophagosome number were evaluated. In vitro, cell viability, autolysosome number, and relationship between miR-143 and ATG2B were determined. miR-143, ATG2B and autophagy-related protein (Beclin-1, p62 and LC3I/LC3II) levels were evaluated in rats and cells. GHS mitigated small intestinal pathological injury and decreased D-lactic acid level for septic rats. Additionally, GHS elevated tight junction protein expressions, ATG2B, Beclin-1 and LC3I/LC3II levels, and autophagosome number, but reduced miR-143 and p62 levels for septic rats. However, miR-143 overexpression presented the opposite results. Consistently, cellular experiments found that GHS increased cell viability, autolysosome number, and presented similar results for miR-143, ATG2B and autophagy-related protein levels for lipopolysaccharides-exposed cells. Additionally, ATG2B directly targeted miR-143 in IEC-6 cells. Both animal and cellular experiments found the effects of GHS on sepsis-induced small intestinal barrier damage were reversed by miR-143 overexpression. GHS may improve small intestinal barrier damage in sepsis through miR-143/ATG2B-mediated autophagy, indicating miR-143/ATG2B was an underlying therapeutic target for sepsis.
Copyright: © 2025 Liu et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures


Similar articles
-
LncRNA GAS5 ameliorates intestinal barrier injury by targeting the miR-223-3p/FBXW7 axis and inactivating NF-κB signaling in vitro and in vivo.J Pathol. 2025 Sep;267(1):25-39. doi: 10.1002/path.6440. Epub 2025 Jul 28. J Pathol. 2025. PMID: 40719162
-
Effects of Acute Abdomen III on Sepsis-Induced Intestinal Damage in a Rat Model.J Microbiol Biotechnol. 2025 Jun 26;35:e2412067. doi: 10.4014/jmb.2412.12067. J Microbiol Biotechnol. 2025. PMID: 40582762 Free PMC article.
-
[Effect of Wenyang Zhenshuai Granules on autophagy and apoptosis of myocardial cells in septic rats via regulating miR-132-3p/UCP2 expression].Zhongguo Zhong Yao Za Zhi. 2023 Jun;48(11):3066-3073. doi: 10.19540/j.cnki.cjcmm.20230216.701. Zhongguo Zhong Yao Za Zhi. 2023. PMID: 37381965 Chinese.
-
Systemic treatments for metastatic cutaneous melanoma.Cochrane Database Syst Rev. 2018 Feb 6;2(2):CD011123. doi: 10.1002/14651858.CD011123.pub2. Cochrane Database Syst Rev. 2018. PMID: 29405038 Free PMC article.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2017 Dec 22;12(12):CD011535. doi: 10.1002/14651858.CD011535.pub2. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2020 Jan 9;1:CD011535. doi: 10.1002/14651858.CD011535.pub3. PMID: 29271481 Free PMC article. Updated.
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

