Effect of driving pressure-guided positive end-expiratory pressure on respiratory mechanics and clinical outcomes in surgical patients: a systematic review and meta-analysis of randomized controlled trials
- PMID: 40781750
- PMCID: PMC12337742
- DOI: 10.1080/07853890.2025.2543978
Effect of driving pressure-guided positive end-expiratory pressure on respiratory mechanics and clinical outcomes in surgical patients: a systematic review and meta-analysis of randomized controlled trials
Abstract
Background: Intraoperative driving pressure-guided positive end-expiratory pressure (PEEPdp) is effective for reducing postoperative pulmonary complications (PPCs). However, its impact on respiratory mechanics and clinical outcomes requires further elaboration.
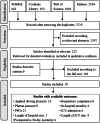
Methods: PubMed, the Cochrane Library, Web of Science and Embase were searched from inception to May 2024 for randomized controlled trials (RCTs) comparing the effect of PEEPdp with conventional fixed positive end-expiratory pressure (PEEP) in patients undergoing surgery. The primary outcomes were the effects on the driving pressure (DP), static respiratory compliance and plateau pressure (Pplat). Secondary outcomes included the effects on common clinical outcomes and the incidence of PPCs. Risk ratios or mean differences were pooled using fixed- or random-effects models.
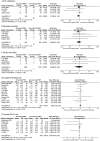
Results: Nineteen RCTs involving 3744 patients were included. The mean of PEEPdp was 8.2 cmH2O with 95% CI from 7 cmH2O to 9.5 cmH2O, while the median of PEEP in the conventional group was 5 cmH2O with an interquartile range of 1 cmH2O. Patients in the PEEPdp group were ventilated with lower DP (mean: 10 cmH2O, 95% CI [8.8, 11.1] vs. mean: 11.9 cmH2O, 95% CI [10.6, 13.3]; p < .00001), and increased respiratory compliance (mean: 46.4 ml/cmH2O, 95% CI [42.1, 50.7] vs. mean: 39 ml/cmH2O, 95% CI [35.2, 42.8]; p < .0001) with nonsignificant Pplat. PEEPdp did not significantly affect intensive care unit (ICU) admission, mortality or length of hospital and ICU stay (p > .05), but it reduced the incidence of PPCs (p = .001). The benefits were especially evident in patients undergoing abdominal surgery, those with DP less than 10 cmH2O or those with PEEPdp ranging from 5 to 10 cmH2O or when PEEPdp was titrated via a stepwise increase method (p < .05).
Conclusions: PEEPdp allows for ventilation with lower DP, improved static respiratory compliance and fewer PPCs. No significant effects were observed on broader clinical outcomes per current data.
Keywords: Respiratory mechanics; driving pressure; intraoperative lung protective ventilation; lung injury; positive end-expiratory pressure.
Conflict of interest statement
No potential conflict of interest was reported by the author(s).
Figures

Similar articles
-
Respiratory muscle training for multiple sclerosis.Cochrane Database Syst Rev. 2017 Dec 21;12(12):CD009424. doi: 10.1002/14651858.CD009424.pub2. Cochrane Database Syst Rev. 2017. PMID: 29267988 Free PMC article.
-
Positioning for acute respiratory distress in hospitalised infants and children.Cochrane Database Syst Rev. 2022 Jun 6;6(6):CD003645. doi: 10.1002/14651858.CD003645.pub4. Cochrane Database Syst Rev. 2022. PMID: 35661343 Free PMC article.
-
Adjustment of positive end-expiratory pressure based on body mass index during general anaesthesia: a randomised controlled trial.Anaesthesia. 2025 Jun 23. doi: 10.1111/anae.16656. Online ahead of print. Anaesthesia. 2025. PMID: 40551551
-
Intravenous magnesium sulphate and sotalol for prevention of atrial fibrillation after coronary artery bypass surgery: a systematic review and economic evaluation.Health Technol Assess. 2008 Jun;12(28):iii-iv, ix-95. doi: 10.3310/hta12280. Health Technol Assess. 2008. PMID: 18547499
-
Continuous positive airway pressure (CPAP) during the postoperative period for prevention of postoperative morbidity and mortality following major abdominal surgery.Cochrane Database Syst Rev. 2014 Aug 1;2014(8):CD008930. doi: 10.1002/14651858.CD008930.pub2. Cochrane Database Syst Rev. 2014. PMID: 25081420 Free PMC article.
References
-
- Fernandez-Bustamante A, Frendl G, Sprung J, et al. Postoperative pulmonary complications, early mortality, and hospital stay following noncardiothoracic surgery: a multicenter study by the perioperative research network investigators. JAMA Surg. 2017;152(2):157–166. doi: 10.1001/jamasurg.2016.4065. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
