Combining bedside index of severity in acute pancreatitis (BISAP) and Charlson comorbidity index improves early risk stratification in biliary acute pancreatitis
- PMID: 40783427
- PMCID: PMC12335518
- DOI: 10.1038/s41598-025-15048-y
Combining bedside index of severity in acute pancreatitis (BISAP) and Charlson comorbidity index improves early risk stratification in biliary acute pancreatitis
Abstract
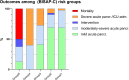
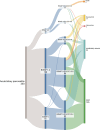
Risk stratification in acute pancreatitis (AP) remains a clinical challenge. Because AP populations are diverse, focusing on one etiology might reveal interesting insights concerning predictors of outcomes. In this retrospective multicenter cohort study, all patients with biliary AP admitted between 2018 and 2021 were included. Predictors of clinical outcomes - including severity, ICU-admission, complications, and 90-day mortality - were assessed. In total, 217 biliary AP patients, mean age 65.9 years (SD 17.4), 49.3% female, were included, with a median length of stay 7 days (IQR 4;11). BISAP scores were 0 in 30.0%, 1-2 in 63.5%, and 3-5 in 6.4% of patients. Higher BISAP and Charlson comorbidity index (CCI) were significantly associated with worse outcomes, including ICU admission, persistent organ dysfunction, and mortality (p < 0.001). When combined, BISAP and CCI identified five risk groups with progressively increasing rates of complications and mortality. Notably, 41.1% of patients fell into the lowest risk group, with only 2 ICU admissions, and with an uncomplicated course in 97.6% of cases, supporting potential early discharge. Mortality in the very-high risk group (BISAP 3-5, CCI ≥ 6) was 50%. The combination (BISAP-C) enhances early prognostication in biliary AP and may guide individualized management and healthcare resource utilization.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Competing interests: The authors declare no competing interests. Disclosure: The authors have no relevant financial or non-financial interests to disclose. This project was supported by Forschungsimpulse [project ID: SF_0046 and project ID: RTO_0028], a program of Karl Landsteiner University of Health Sciences funded by the Federal Government of Lower Austria.
Figures
Similar articles
-
Understanding Etiopathogenesis and Clinical Outcomes in Acute Pancreatitis: An Experience From a Tertiary Care Teaching Hospital in Andhra Pradesh.Cureus. 2025 Jul 14;17(7):e87913. doi: 10.7759/cureus.87913. eCollection 2025 Jul. Cureus. 2025. PMID: 40809623 Free PMC article.
-
Association between magnesium sulfate administration and short-term mortality in acute pancreatitis patients admitted to the ICU: a retrospective cohort study based on the MIMIC-III and MIMIC–IV database.Magnes Res. 2025 Dec 1;38(1):26-39. doi: 10.1684/mrh.2025.0544. Magnes Res. 2025. PMID: 40626736 French.
-
Evaluation of the PAN-PROMISE Symptom Scale in a Randomized Controlled Trial of Fluid Resuscitation in Acute Pancreatitis.Am J Gastroenterol. 2025 Jun 5;120(8):1852-1859. doi: 10.14309/ajg.0000000000003570. Am J Gastroenterol. 2025. PMID: 40471836 Clinical Trial.
-
Use of proton pump inhibitors improves outcomes in mild acute pancreatitis: A nationwide cohort study.Medicine (Baltimore). 2024 Apr 5;103(14):e37694. doi: 10.1097/MD.0000000000037694. Medicine (Baltimore). 2024. PMID: 38579028 Free PMC article. Review.
-
The Value of BISAP Score for Predicting Mortality and Severity in Acute Pancreatitis: A Systematic Review and Meta-Analysis.PLoS One. 2015 Jun 19;10(6):e0130412. doi: 10.1371/journal.pone.0130412. eCollection 2015. PLoS One. 2015. PMID: 26091293 Free PMC article.
References
-
- Andersson, B. et al. Acute pancreatitis–costs for healthcare and loss of production. Scand. J. Gastroenterol.48 (12), 1459–1465 (2013). - PubMed
-
- Lankisch, P. G., Karimi, M., Bruns, A., Maisonneuve, P. & Lowenfels, A. B. Temporal trends in incidence and severity of acute pancreatitis in Luneburg county, germany: a population-based study. Pancreatology9 (4), 420–426 (2009). - PubMed
-
- Loosen, S. H. et al. Current epidemiological trends and in-hospital mortality of acute pancreatitis in germany: a systematic analysis of standardized hospital discharge data between 2008 and 2017. Z. Gastroenterol.60 (3), 310–319 (2022). - PubMed
-
- Tenner, S. et al. American college of gastroenterology guidelines: management of acute pancreatitis. Am. J. Gastroenterol.119 (3), 419–437 (2024). - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

