The prevalence of pediatric nosocomial fungal infections
- PMID: 40785725
- PMCID: PMC12331464
- DOI: 10.18502/ijm.v17i4.19258
The prevalence of pediatric nosocomial fungal infections
Abstract
Background and objectives: The aim of this study was to identify the incidence of nosocomial fungal infections in pediatric patients and evaluate the etiological agents, risk factors, and sites of infections.
Materials and methods: Clinical samples were cultured to assess fungal colonization. When fungal nosocomial infections were suspected according to the European Organization for Research and Treatment of Cancer criteria, clinical samples were evaluated using direct microscopic, culture, and molecular methods. Susceptibility patterns of the isolates were evaluated according to the Clinical and Laboratory Standard Institute.
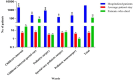
Results: From the 1450 patients, 190 cases (5.5%) were evaluated for nosocomial fungal infections. Candida colonization was observed in 35 (18.4%) patients. The rate of nosocomial fungal infections in pediatrics was 2.69% (12 cases with proven and 27 cases with probable infections, 39/1450). Bloodstream and lungs were the frequent infected sites of patients' body. Aspergillus species (Aspergillus flavus and Aspergillus fumigatus), Candida species (Candida albicans, Candida parapsilosis, Candida glabrata) and Mucorales were the etiologic agents of infections. Caspofungin and luliconazole were effective antifungal agents for isolated fungi. The rate of mortality in infected patients suffering from proven and probable infections was 15.4% (6/39 cases).
Conclusion: Due to the high mortality rates of fungal infections in pediatrics, it is essential to identify modifiable risk factors, and implement control measures along with early detection techniques in pediatric populations.
Keywords: Aspergillus; Candida; Colonization; Fungal drug resistance; Fungal infection; Pediatrics.
Copyright © 2025 The Authors. Published by Tehran University of Medical Sciences.
Figures
Similar articles
-
Epidemiology and antifungal susceptibility of fungal infections from 2018 to 2021 in Shandong, eastern China: A report from the SPARSS program.Indian J Med Microbiol. 2024 Jan-Feb;47:100518. doi: 10.1016/j.ijmmb.2023.100518. Epub 2023 Dec 5. Indian J Med Microbiol. 2024. PMID: 38016503
-
Multidrug-Resistant Candida in Bloodstream Infections: A Growing Concern in Indian Healthcare.Cureus. 2025 Jun 5;17(6):e85420. doi: 10.7759/cureus.85420. eCollection 2025 Jun. Cureus. 2025. PMID: 40621298 Free PMC article.
-
Antifungal susceptibility profiles of Candida and non-albicans species isolated from pregnant women: implications for emerging antimicrobial resistance in maternal health.Microbiol Spectr. 2025 Jul;13(7):e0078725. doi: 10.1128/spectrum.00787-25. Epub 2025 Jun 2. Microbiol Spectr. 2025. PMID: 40454865 Free PMC article.
-
Antifungal agents for preventing fungal infections in non-neutropenic critically ill patients.Cochrane Database Syst Rev. 2016 Jan 16;2016(1):CD004920. doi: 10.1002/14651858.CD004920.pub3. Cochrane Database Syst Rev. 2016. PMID: 26772902 Free PMC article.
-
Development and validation of a risk model for identification of non-neutropenic, critically ill adult patients at high risk of invasive Candida infection: the Fungal Infection Risk Evaluation (FIRE) Study.Health Technol Assess. 2013 Feb;17(3):1-156. doi: 10.3310/hta17030. Health Technol Assess. 2013. PMID: 23369845 Free PMC article.
References
-
- Fisher BT, Robinson PD, Lehrnbecher T, Steinbach WJ, Zaoutis TE, Phillips B, et al. Risk factors for invasive fungal disease in Pediatric cancer and Hematopoietic stem cell transplantation: A systematic review. J Pediatric Infect Dis Soc 2018; 7: 191–198. - PubMed
-
- Suleyman G, Alangaden GJ. Nosocomial fungal infections: Epidemiology, infection control, and Prevention. Infect Dis Clin North Am 2016; 30: 1023–1052. - PubMed
-
- Zingg W, Hopkins S, Gayet-Ageron A, Holmes A, Sharland M, Suetens C, et al. Health-care-associated infections in neonates, children, and adolescents: an analysis of paediatric data from the European centre for disease Prevention and control point-prevalence survey. Lancet Infect Dis 2017; 17: 381–389. - PubMed
LinkOut - more resources
Full Text Sources