Risk factors for rehospitalization after trauma: a follow-up study
- PMID: 40788478
- PMCID: PMC12339642
- DOI: 10.1007/s00068-025-02944-1
Risk factors for rehospitalization after trauma: a follow-up study
Abstract
Introduction: Unplanned rehospitalizations represent a heavy burden to patients, their families, and an economic burden on the healthcare system.
Objective: The aim of this study was to examine patterns of trauma-related rehospitalization within 7, 30, 60, and 90 days after initial discharge, and to assess the association between patient age and the risk of rehospitalization, while adjusting for relevant demographic and clinical factors.
Methods: This retrospective cohort study links two national databases: The Israeli National Trauma Registry and the Ministry of Health's hospitalization database. Univariate analyses (χ2 tests) were performed to identify factors associated with rehospitalization at 7, 30, 60, and 90 days post-discharge. Variables significantly associated in univariate analysis were entered into separate multivariable Generalized Estimating Equations (GEE) models for each time point.
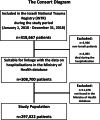
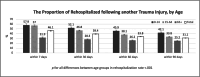
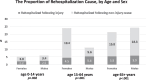
Results: The study included 297,022 trauma patients (median age 34 years [IQR: 14-67]; 59.3% male). Most injuries were non-penetrating (88.8%), and the majority were classified as mild (ISS 1-8, 64.9%). Falls (53.0%) and road traffic accidents (23.8%) were the most common injury mechanisms. The most affected age group was 19-54 years (34.3%), and 71.3% of patients were from the Jewish population group. The rate was 4.4% for rehospitalized within seven days, 9.2% within 30 days, 12.3% within 60 days, and 14.7% within 90 days. In multivariable analysis, a clear association was observed between increasing age and higher odds of rehospitalization following discharge for trauma. Compared to the reference group (ages 0-4), older patients exhibited substantially elevated odds across all follow-up periods. For instance, patients aged 75-84 had odds ratios (ORs) of 4.39, 4.75, 4.95, and 3.33 for rehospitalization within 7, 30, 60, and 90 days, respectively. Similarly, individuals aged 85 + had ORs of 5.42, 5.68, 6.0, and 3.47, respectively. Higher odds of rehospitalization peaked at 60 days post-discharge and decreased by 90 days, suggesting possible stabilization.
Conclusions and recommendations: Comprehensive discharge planning and a care transition system for trauma patients should involve a multidisciplinary team to address the patient's specific condition and rehospitalization risk factors, especially among older adults hospitalized following a fall.
Keywords: Injury; Rehospitalization; Trauma; Trauma registry.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethical approval: This study was conducted in accordance with the Declaration of Helsinki and approved by the Ethical Committee of the Sheba Medical Center (#SMC-5424–18) and the Ministry of Health (#20187712), which determined that informed consent was not required due to the use of anonymous data. Consent to participate: Not applicable. Competing interests: The authors declare no competing interests.
Figures

Similar articles
-
Falls prevention interventions for community-dwelling older adults: systematic review and meta-analysis of benefits, harms, and patient values and preferences.Syst Rev. 2024 Nov 26;13(1):289. doi: 10.1186/s13643-024-02681-3. Syst Rev. 2024. PMID: 39593159 Free PMC article.
-
Comparison of Two Modern Survival Prediction Tools, SORG-MLA and METSSS, in Patients With Symptomatic Long-bone Metastases Who Underwent Local Treatment With Surgery Followed by Radiotherapy and With Radiotherapy Alone.Clin Orthop Relat Res. 2024 Dec 1;482(12):2193-2208. doi: 10.1097/CORR.0000000000003185. Epub 2024 Jul 23. Clin Orthop Relat Res. 2024. PMID: 39051924
-
Increasing Trends of Pediatric Thoracic and Lumbar Spine Fractures in the United States from 2004 to 2023: A 20-year National Injury Review Depicting Shifts in Mechanisms of Injury.Clin Orthop Relat Res. 2025 Feb 25;483(8):1542-1553. doi: 10.1097/CORR.0000000000003421. Clin Orthop Relat Res. 2025. PMID: 40036050
-
High Risk of Readmission After THA Regardless of Functional Status in Patients Discharged to Skilled Nursing Facility.Clin Orthop Relat Res. 2024 Jul 1;482(7):1185-1192. doi: 10.1097/CORR.0000000000002950. Epub 2024 Jan 16. Clin Orthop Relat Res. 2024. PMID: 38227380 Free PMC article.
-
Home treatment for mental health problems: a systematic review.Health Technol Assess. 2001;5(15):1-139. doi: 10.3310/hta5150. Health Technol Assess. 2001. PMID: 11532236
References
-
- Fallatah HI, Bajunaid NF, Jawa HA, Qari YA, Bazarah SM, Aljohaney AA, et al. Readmission within 30-day as a key indicator for academic hospital performance: Rate and risk factors. Saudi Journal of Internal Medicine. 2019;9:29–35.
-
- Moore L, Stelfox HT, Turgeon AF, Nathens AB, Lavoie A, Bourgeois G, et al. Derivation and validation of a quality indicator for 30-day unplanned hospital readmission to evaluate trauma care. J Trauma Acute Care Surg. 2014;76:1310–6. - PubMed
-
- Copertino LM, McCormack JE, Rutigliano DN, Huang EC, Shapiro MJ, Vosswinkel JA, et al. Early unplanned hospital readmission after acute traumatic injury: The experience at a state-designated level-I trauma center. Am J Surg. 2015;209:268–73. - PubMed
-
- Marcin JP, Romano PS. Impact of between-hospital volume and within-hospital volume on mortality and readmission rates for trauma patients in California. Crit Care Med. 2004;32:1477–83. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

