Limiting endosomal damage sensing reduces inflammation triggered by lipid nanoparticle endosomal escape
- PMID: 40789922
- PMCID: PMC12352612
- DOI: 10.1038/s41565-025-01974-5
Limiting endosomal damage sensing reduces inflammation triggered by lipid nanoparticle endosomal escape
Abstract
Lipid nanoparticles (LNPs) have emerged as the dominant platform for RNA delivery, but they induce severe inflammation. Here we show that LNPs' hallmark feature, endosomal escape, which is necessary for RNA expression, also triggers inflammation by causing endosomal membrane damage. Large, irreparable, endosomal holes are recognized by cytosolic proteins called galectins, which regulate downstream inflammation. We find that inhibition of galectins abrogates LNP-associated inflammation, both in vitro and in vivo. Moreover, we show that a unique class of ionizable lipids can create smaller endosomal holes, reparable by the endosomal sorting complex required for transport (ESCRT) pathway. Such lipids can produce high expression from cargo messenger RNA with minimal inflammation. Finally, we show that both galectin inhibition or ESCRT-recruiting ionizable lipids allow for treatment of highly inflammatory disease models by therapeutic mRNAs. These strategies should lead to safer non-inflammatory LNPs that can be generally used to treat inflammatory diseases.
© 2025. The Author(s), under exclusive licence to Springer Nature Limited.
Conflict of interest statement
Competing interests: The authors declare no competing interests.
Figures




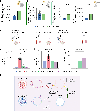
References
-
- Verma M et al. The landscape for lipid-nanoparticle-based genomic medicines. Nat. Rev. Drug Discov. 22, 349–350 (2023). - PubMed
MeSH terms
Substances
Grants and funding
- R01 HL160694/HL/NHLBI NIH HHS/United States
- 1F31AG077874-01/U.S. Department of Health & Human Services | National Institutes of Health (NIH)
- K08 HL150226/HL/NHLBI NIH HHS/United States
- R01 HL164594/HL/NHLBI NIH HHS/United States
- R01HL60694/U.S. Department of Health & Human Services | NIH | National Heart, Lung, and Blood Institute (NHLBI)
- F31 AG077874/AG/NIA NIH HHS/United States
- R41NS130812/U.S. Department of Health & Human Services | National Institutes of Health (NIH)
- R01 NS 131279/U.S. Department of Health & Human Services | NIH | National Institute of Neurological Disorders and Stroke (NINDS)
- R01 NS131279/NS/NINDS NIH HHS/United States
- 24PRE1195406/American Heart Association (American Heart Association, Inc.)
- F31HL154662/U.S. Department of Health & Human Services | National Institutes of Health (NIH)
- F30 AI179472/AI/NIAID NIH HHS/United States
- R01 HL157189/HL/NHLBI NIH HHS/United States
- 5K08HL150226/U.S. Department of Health & Human Services | National Institutes of Health (NIH)
- R01DA057337/U.S. Department of Health & Human Services | NIH | National Institute on Drug Abuse (NIDA)
- R61DA058501/U.S. Department of Health & Human Services | NIH | National Institute on Drug Abuse (NIDA)
- F31 HL154662/HL/NHLBI NIH HHS/United States
- R61 DA058501/DA/NIDA NIH HHS/United States
- 23PRE1014444/American Heart Association (American Heart Association, Inc.)
- R41 NS130812/NS/NINDS NIH HHS/United States
- R01HL164594/U.S. Department of Health & Human Services | NIH | National Heart, Lung, and Blood Institute (NHLBI)
- R01 DA057337/DA/NIDA NIH HHS/United States
- R01 HL153510/HL/NHLBI NIH HHS/United States
- R01 HL157189/HL/NHLBI NIH HHS/United States
- R01 HL157189/HL/NHLBI NIH HHS/United States
- R01 HL157189/HL/NHLBI NIH HHS/United States
LinkOut - more resources
Full Text Sources

