Characteristics and risk factors for medical malpractice among obstetric and gynecologic physicians in China
- PMID: 40797251
- PMCID: PMC12345042
- DOI: 10.1186/s12913-025-13225-3
Characteristics and risk factors for medical malpractice among obstetric and gynecologic physicians in China
Abstract
Background: Limited information is available on malpractice claims against obstetricians and gynecologists in China. This study identifies risk factors associated with malpractice and explores the correlation between the hospital characteristics and medical errors in obstetrics and gynecology.
Methods: This observational study analyzed all obstetric and gynecologic malpractice claims submitted to the Chinese Medical Association (CMA) from 2016 to 2023. Data were extracted from the CMA appraisal reports, including hospital type (general or specialized), tier (primary, secondary, or tertiary), ownership (public or private), primary department involved (obstetrics or gynecology), and detailed case characteristics. Malpractice claims were categorized by the type of medical error. Univariate and multivariate analyses were conducted to assess associations between medical errors and personal, administrative, and professional factors.
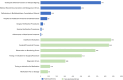
Results: Among the 3,719 cases evaluated by the CMA, 3,676 were confirmed as malpractice. Nonfatal disability occurred in 1,339 cases (36.4%), and death occurred in 735 cases (20.0%). Specialized hospitals had a lower risk of malpractice-related death compared with general hospitals (odds ratio [OR] = 0.785; 95% confidence interval [CI] = 0.637-0.967). Private hospitals showed a reduced risk of severe nonfatal disability compared to public hospitals (OR 0.572; 95% CI 0.361-0.907). Secondary and tertiary hospitals were associated with a higher risk of severe nonfatal disability (OR 1.698 and 1.835, respectively; 95% CI 1.084-2.658 and 1.121-3.004) but a lower risk of primary liability compared with primary hospitals (OR 0.783 and 0.527; 95% CI 0.635-0.965 and 0.419-0.664). Compared with gynecology departments, obstetric cases presented a higher risk of malpractice-related death (2.866; 2.347-3.501) but a lower risk of primary liability (0.643; 0.559-0.740). Compared with public hospitals, private hospitals had more credential-related errors but fewer issues with informed consent and documentation. Obstetric cases more often involved errors in procedural timing, monitoring, and evaluation, whereas gynecologic cases had a higher frequency of surgical process errors (all P < 0.001).
Conclusions: This study provides the first nationwide analysis of obstetric and gynecologic malpractice claims in China. Strengthening grassroots and private hospitals and refining the hierarchical medical system may improve patient safety and healthcare sustainability.
Trial registration: Not available.
Keywords: China; Disability; Malpractice; Obstetrics and gynecology; Technical error.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: Not applicable. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures
Similar articles
-
Prescription of Controlled Substances: Benefits and Risks.2025 Jul 6. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2025 Jul 6. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 30726003 Free Books & Documents.
-
The Perinatal Committee report: Review of the progress of obstetric healthcare in Japan.J Obstet Gynaecol Res. 2025 Jul;51(7):e16354. doi: 10.1111/jog.16354. J Obstet Gynaecol Res. 2025. PMID: 40690975 Free PMC article. Review.
-
Healthcare utilization in the departments of obstetrics and gynecology during the first two years of the COVID-19 pandemic: time series analysis in Jining, China.BMC Public Health. 2025 Mar 13;25(1):996. doi: 10.1186/s12889-025-22160-1. BMC Public Health. 2025. PMID: 40082827 Free PMC article.
-
Sexual Harassment and Prevention Training.2024 Mar 29. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2024 Mar 29. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 36508513 Free Books & Documents.
-
[Volume and health outcomes: evidence from systematic reviews and from evaluation of Italian hospital data].Epidemiol Prev. 2013 Mar-Jun;37(2-3 Suppl 2):1-100. Epidemiol Prev. 2013. PMID: 23851286 Italian.
References
-
- Corina I, Abram M, Halperin D. The patient’s role in patient safety. Obstet Gynecol Clin North Am. 2019;46(2):215–25. - PubMed
-
- Glaser LM, Alvi FA, Milad MP. Trends in malpractice claims for obstetric and gynecologic procedures, 2005 through 2014. Am J Obstet Gynecol. 2017;217(3):340.e1-.e6. - PubMed
-
- Zhang K, Li Y, Fan F, Liu X, Deng ZH. Court decisions on medical malpractice in China after the new tort liability law. Am J Forensic Med Pathol. 2016;37(3):149–51. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources