Efficacy and safety of non-pharmacological therapies for primary insomnia: a network meta-analysis
- PMID: 40808922
- PMCID: PMC12344310
- DOI: 10.3389/fneur.2025.1607903
Efficacy and safety of non-pharmacological therapies for primary insomnia: a network meta-analysis
Abstract
Background: Primary insomnia (PI) is a prevalent sleep disorder that significantly impacts quality of life. While pharmacological treatments are common, concerns about side effects and dependency have led to increased interest in non-pharmacological alternatives. This study systematically evaluates the efficacy and safety of various non-pharmacological therapies for adult PI through a network meta-analysis, providing evidence-based guidance for clinicians.
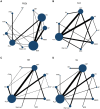
Methods: We analyzed 53 randomized controlled trials (RCTs) involving 4,181 adults with PI. The included studies assessed 11 non-pharmacological interventions, such as acupuncture, acupressure, cupping therapy, and cognitive behavioral therapy (CBT), alongside control groups (e.g., placebo, waitlist, and pharmacological comparators). Primary outcomes included the Pittsburgh Sleep Quality Index (PSQI), total sleep time (TST), sleep efficiency (SE), and sleep latency (SL). Data synthesis was performed using STATA 17 software with a random-effects model, and evidence quality was appraised using the GRADE framework.
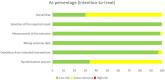
Results: Pooled analyses revealed that all seven non-pharmacological therapies significantly improved PI outcomes compared to controls. Acupuncture reduced PSQI scores by -2.71 points (95% confidence interval (CI): -4.94 to -0.49) versus waitlist, while acupuncture showed a - 1.81 point reduction (95% CI: -2.93 to -0.68). For SE, acupressure and CBT increased SE by 1.48% (95% CI: 0.56-2.39) and 1.34% (95% CI: 0.70-1.98), respectively, compared to SH. Notably, CBT and acupressure shortened SL by approximately 10 min (e.g., CBT: -10.15 min, 95% CI: -11.79 to -8.52 vs. benzodiazepines), while acupressure extended TST by 2.07 h (95% CI: 0.46-3.68). SUCRA rankings identified CBT as the most effective for reducing SL (85.8% probability) and improving SE (89.2%), whereas acupuncture excelled in increasing TST (84.8%). Adverse events were infrequent and mild, primarily limited to transient localized reactions in acupuncture studies.
Conclusion: This study demonstrates that non-pharmacological therapies are effective and safe in managing PI, with CBT, acupuncture, and acupressure emerging as optimal choices for specific sleep parameters. These findings advocate non-pharmacological interventions into clinical practice and offer clinicians valuable insights for selecting appropriate treatment modalities for PI management. However, study limitations like heterogeneity and small sample sizes highlight the need for larger, well-designed RCTs. Future studies should use standardized measures for more specific insomnia assessment.
Keywords: acupressure; acupuncture; cognitive behavioral therapy; cupping therapy; primary insomnia.
Copyright © 2025 Zhang, Liu, Yang, Zhu, Yang, Li, Yan, Liu, Yue, Li, Li, Xu and Jiang.
Conflict of interest statement
Q-hZ and J-hY were employed by Shenzhen Frontiers in Chinese Medicine Research Co., Ltd. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


References
-
- Roth T, Coulouvrat C, Hajak G, Lakoma MD, Sampson NA, Shahly V, et al. Prevalence and perceived health associated with insomnia based on DSM-IV-TR; ICD-10; and research diagnostic criteria/ICSD-2 criteria: results from the American insomnia survey. Biol Psychiatry. (2011) 69:592–600. doi: 10.1016/j.biopsych.2010.10.023, PMID: - DOI - PubMed
-
- Qaseem A, Kansagara D, Forciea MA, Cooke M, Denberg TD, for the Clinical Guidelines Committee of the American College of Physicians* . Management of chronic insomnia disorder in adults: a clinical practice guideline from the American College of Physicians. Ann Intern Med. (2016) 165:125–33. doi: 10.7326/M15-2175, PMID: - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

