The Impact of Post-Operative Phrenic Nerve Dysfunction on Lung Function Parameters and Long-Term Outcomes After Lung Transplantation
- PMID: 40809907
- PMCID: PMC12343345
- DOI: 10.3389/ti.2025.14691
The Impact of Post-Operative Phrenic Nerve Dysfunction on Lung Function Parameters and Long-Term Outcomes After Lung Transplantation
Abstract
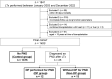
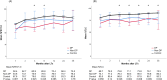
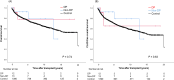
A rare but important complication after lung transplantation (LTx) is postoperative phrenic nerve dysfunction (PND). Diaphragmatic plication (DP) is a well-established treatment option for PND, however, the long-term effect of PND and DP on lung function parameters and survival after LTx are currently unknown. We retrospectively reviewed 1400 LTx recipients transplanted at Medical University of Vienna between 01/2003 and 12/2022. Fluoroscopy and/or phrenic nerve conduction studies confirmed PND when chest radiographs after extubation showed a unilateral heightened diaphragm. We identified 25 patients with post-operative PND, of whom 12 underwent DP. The remaining 1,375 patients served as a control group. Median ICU-stay and hospital-stay were significantly longer in the PND groups (DP: 20 and 57 days; non-DP: 27 and 43 days; control group: 7 and 25 days; P = 0.001/P < 0.001). PND led to consistently lower %TLC in lung function tests performed within the first three years after LTx. DP was associated with lower %FEV1.0 early after LTx but it aligned to %FEV1.0 of the other groups during follow-up. Although PND significantly affected postoperative recovery after LTx, it did not impair long-term survival outcomes.
Keywords: diaphragmatic plication; lung function parameters; lung transplantation; phrenic nerve dysfunction; surgery.
Copyright © 2025 Nakanishi, Hillebrand, Schweiger, Schwarz, Taghavi, Jaksch, Benazzo, Chen-Yoshikawa and Hoetzenecker.
Conflict of interest statement
KN was supported by a fellowship grant from the Uehara Memorial Foundation (Tokyo, Japan) in 2022. The funding source had no role in the design, practice, or analysis of this study. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Phrenic nerve dysfunction after heart-lung and lung transplantation.J Heart Lung Transplant. 2004 Jan;23(1):105-9. doi: 10.1016/s1053-2498(03)00068-8. J Heart Lung Transplant. 2004. PMID: 14734134
-
Phrenic Nerve Reconstruction in Pediatric Diaphragm Paralysis: Outcomes and Techniques.Eur J Pediatr Surg. 2025 Aug;35(4):302-308. doi: 10.1055/a-2536-4405. Epub 2025 Feb 11. Eur J Pediatr Surg. 2025. PMID: 39933731
-
[Effect of transcutaneous phrenic nerve stimulation in preventing ventilator-induced diaphragmatic dysfunction in invasive mechanically ventilated patients].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2025 Apr;37(4):343-347. doi: 10.3760/cma.j.cn121430-20240111-00037. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2025. PMID: 40814706 Clinical Trial. Chinese.
-
Prenatal interventions for congenital diaphragmatic hernia for improving outcomes.Cochrane Database Syst Rev. 2015 Nov 27;2015(11):CD008925. doi: 10.1002/14651858.CD008925.pub2. Cochrane Database Syst Rev. 2015. PMID: 26611822 Free PMC article.
-
Intravenous magnesium sulphate and sotalol for prevention of atrial fibrillation after coronary artery bypass surgery: a systematic review and economic evaluation.Health Technol Assess. 2008 Jun;12(28):iii-iv, ix-95. doi: 10.3310/hta12280. Health Technol Assess. 2008. PMID: 18547499
References
-
- Thabut G, Christie JD, Ravaud P, Castier Y, Brugière O, Fournier M, et al. Survival after Bilateral versus Single Lung Transplantation for Patients with Chronic Obstructive Pulmonary Disease: A Retrospective Analysis of Registry Data. Lancet (2008) 371:744–51. 10.1016/S0140-6736(08)60344-X - DOI - PubMed
-
- Sano Y, Oto T, Toyooka S, Yamane M, Okazaki M, Date H. Phrenic Nerve Paralysis Following Lung Transplantation. Kyobu Geka (2007) 60:993–7. PMID: 17926903. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

