Neuroimaging for neurovascular complications of traumatic brain injury
- PMID: 40826095
- PMCID: PMC12362949
- DOI: 10.1186/s13054-025-05586-2
Neuroimaging for neurovascular complications of traumatic brain injury
Abstract
Background: Traumatic brain injury typically causes extra-axial and/or intra-axial bleeding including subarachnoid hemorrhage, intraparenchymal hemorrhage, subdural hematomas and epidural hematomas. Less commonly, trauma can cause cerebrovascular complications, which involve either the arterial or the venous side. Because of the rarity of these pathological conditions, guidelines and recommendations for their management are still controversial.
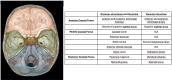
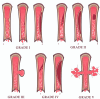
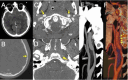
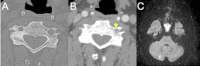
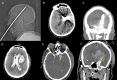
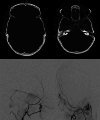
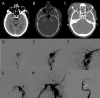
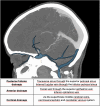
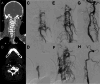
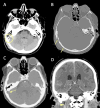
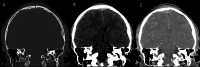
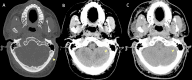
Main body: The objective of this work is to describe the possible cerebrovascular complications of critically ill traumatic brain injured patients and to understand the most common underlying mechanisms and radiological features as well as their management. A variety of pathological entities will be addressed, such as post-traumatic aneurysms, carotid-cavernous fistula, arterial occlusion, arterial dissection (in potential association with brain ischemia), as well as arterial rupture/avulsion and post-traumatic venous thrombosis. Neurovascular complications of head trauma vary depending on the traumatic mechanism, on the site of impact and on the osseous structures involved. Early diagnosis is mostly based on Computed Tomography/Computed Tomography Angiography (CT/CTA) whose findings help guide patient management by detecting vascular lesions potentially leading to neurological deterioration. Magnetic resonance imaging may be useful in selected cases. Today Digital Subtraction Angiography (DSA) is mostly a diagnostic problem-solving tool when CTA findings are equivocal but advanced endovascular interventional techniques have improved the therapeutic possibilities in post-traumatic vascular complications. CONCLUSIONS: Neurovascular complications are not common after head trauma but should not be overlooked because they might lead to severe and life-threatening consequences. Early diagnosis, and a multidisciplinary collaboration including neuroradiologists, neurosurgeons and neurointensivists is fundamental in order to prevent and minimize secondary brain damage in this population.
Keywords: Neurocritical care; Neuroimaging; Neurovascular complications; Traumatic brain injury.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: The ethics committee approved the study (reference number register CER Liguria: 340/2022—DB id 12,413). Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures
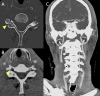
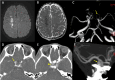
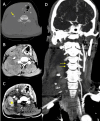
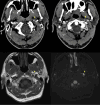
Similar articles
-
Prescription of Controlled Substances: Benefits and Risks.2025 Jul 6. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2025 Jul 6. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 30726003 Free Books & Documents.
-
Elbow Fractures Overview.2025 Jul 7. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2025 Jul 7. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 28723005 Free Books & Documents.
-
Sexual Harassment and Prevention Training.2024 Mar 29. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2024 Mar 29. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 36508513 Free Books & Documents.
-
Management of urinary stones by experts in stone disease (ESD 2025).Arch Ital Urol Androl. 2025 Jun 30;97(2):14085. doi: 10.4081/aiua.2025.14085. Epub 2025 Jun 30. Arch Ital Urol Androl. 2025. PMID: 40583613 Review.
-
The Black Book of Psychotropic Dosing and Monitoring.Psychopharmacol Bull. 2024 Jul 8;54(3):8-59. Psychopharmacol Bull. 2024. PMID: 38993656 Free PMC article. Review.
References
-
- Weber CD, Lefering R, Kobbe P, Horst K, Pishnamaz M, Sellei RM, et al. Blunt cerebrovascular artery injury and stroke in severely injured patients: an international multicenter analysis. World J Surg. 2018;42(7):2043–53. - PubMed
-
- Esnault P, Cardinale M, Boret H, D’Aranda E, Montcriol A, Bordes J, et al. Blunt cerebrovascular injuries in severe traumatic brain injury: incidence, risk factors, and evolution. J Neurosurg. 2017;127(1):16–22. - PubMed
-
- Krings T, Geibprasert S, Lasjaunias PL. Cerebrovascular trauma. Eur Radiol. 2008;18(8):1531–45. - PubMed
-
- Stone DK, Viswanathan VT, Wilson CA. Management of blunt cerebrovascular injury. Curr Neurol Neurosci Rep. 2018;18(12):1–9. - PubMed
-
- Steenburg SD, Sliker CW, Shanmuganathan K, Siegel EL (2010) Imaging evaluation of penetrating neck injuries. Radiographics 30:869–886 - PubMed
Publication types
LinkOut - more resources
Full Text Sources

