Measurement and Sequelae of Neonatal Skin Injuries: A Prospective Diagnostic/Feasibility Study
- PMID: 40827056
- PMCID: PMC12361808
- DOI: 10.1111/iwj.70745
Measurement and Sequelae of Neonatal Skin Injuries: A Prospective Diagnostic/Feasibility Study
Abstract
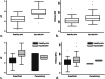
Neonatal skin injuries are common, but location and metric size contribute to inconsistent severity reporting. To date, non-invasive technologies remain unexplored for neonatal injuries. The aim of this study was to assess the feasibility and accuracy of visual assessment against three technologies for injuries to the skin from pressure, stripping and tearing. The prospective diagnostic/feasibility study was conducted for neonates who acquired mechanical force injuries between February-July 2022. Injury measures taken within 72 h of identification were (i) skin injury severity or type pH (5.0-7.5), (ii) laser speckle (perfusion units/mm2), and (iii) imaging app (surface area, cm2). Technology feasibility, clinician-reported acceptability, accuracy, cost and injury sequelae at 6 months post-injury were also collected. A total of 24 neonates (mean (SD)) 34 (5) weeks old and (median (IQR) weight) 1244 (868 to 1740) grams were enrolled. Forty injuries (n = 120 assessments) were completed by visual assessment (100%), 34 (85%) by pH, 30 (75%) with laser speckle and 38 (95%) with the imaging app, respectively. Assessments between clinicians and researchers were inconsistent (n = 29, 72%) and technologies failed for at least 3% of assessments by each respective device. Median injured pH exceeded healthy (average -0.7 of unit), but differences between injured and healthy skin with laser speckle and the app were non-significant. Skin pH had the quickest acquisition (mean (SD) 3.1 (1.6) min) followed by the app (3.2 (2.5) min) and mean acceptability was highest for the imaging app (7.1/10), then pH (6.4/10). Cost per injury was most expensive for the app ($6.65 to $12.82) and lowest for pH ($0.17 to $0.41) per assessment. In conjunction with visual assessment, pH appears objective and cost-effective for intact and injured skin comparison.
Keywords: computer vision; digital application; injury; neonatal skin integrity; wound.
© 2025 The Author(s). International Wound Journal published by Medicalhelplines.com Inc and John Wiley & Sons Ltd.
Conflict of interest statement
D.A. has undertaken consultancy work for NAVI Technologies and 3M unrelated to this work. N.M. reports, Griffith University and the University of Queensland have received on their behalf speaker fees from 3M, investigator‐initiated research grants from Becton Dickinson, Eloquest, Biolife and Cardinal Health, unrelated to this study. F.C. has received speaker fees from Solventum (Formerly 3M). A.U. reports investigator‐initiated research grants paid to her employer from BD, 3M, Medline, Eloquest and Biolife, unrelated to this study. S.H., Ly.C., L.C., M.L., J.H., D.H., P.K., G.X., J.C., R.R., J.B., C.Mc., R.W., and F.C. have no conflicts of interest.
Figures

Similar articles
-
Prescription of Controlled Substances: Benefits and Risks.2025 Jul 6. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2025 Jul 6. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 30726003 Free Books & Documents.
-
Falls prevention interventions for community-dwelling older adults: systematic review and meta-analysis of benefits, harms, and patient values and preferences.Syst Rev. 2024 Nov 26;13(1):289. doi: 10.1186/s13643-024-02681-3. Syst Rev. 2024. PMID: 39593159 Free PMC article.
-
A digital intervention to improve mental health and interpersonal resilience for young people who have experienced online sexual abuse: the i-Minds non-randomised feasibility clinical trial and nested qualitative study.Health Soc Care Deliv Res. 2025 Jul;13(28):1-27. doi: 10.3310/THAL8732. Health Soc Care Deliv Res. 2025. PMID: 40754856
-
Variation within and between digital pathology and light microscopy for the diagnosis of histopathology slides: blinded crossover comparison study.Health Technol Assess. 2025 Jul;29(30):1-75. doi: 10.3310/SPLK4325. Health Technol Assess. 2025. PMID: 40654002 Free PMC article.
-
Acupuncture for neonatal abstinence syndrome in newborn infants.Cochrane Database Syst Rev. 2025 Feb 21;2(2):CD014160. doi: 10.1002/14651858.CD014160.pub2. Cochrane Database Syst Rev. 2025. PMID: 39981752
References
-
- August D. L., Kandasamy Y., Ray R., Lindsay D., and New K., “Fresh Perspectives on Hospital Acquired Neonatal Skin Injury Prevalence From a Multicentre Study: Length of Stay, Acuity and Incomplete Course of Antenatal Steroids,” Journal of Perinatal and Neonatal Nursing 35, no. 3 (2021): 275–283. - PubMed
-
- August D. L., Ray R. A., Kandasamy Y., and New K., “Neonatal Skin Assessments and Injuries: Nomenclature, Workplace Culture and Clinical Opinions‐Method Triangulation a Qualitative Study,” Journal of Clinical Nursing 29, no. 21–22 (2020): 3986–4006. - PubMed
-
- European Pressure Ulcer Advisory Panel NPIAPaPPPIA , Prevention and Treatment of Pressure Ulcers/Inuries Clinical Practice Guideline. The International Guideline, 2019.
Grants and funding
LinkOut - more resources
Full Text Sources

