An Overview on Methods, Evidence, and Study Quality of Health Economic Evaluation Studies for Independently Usable Digital Health Apps: Rapid Review
- PMID: 40829140
- PMCID: PMC12364420
- DOI: 10.2196/68349
An Overview on Methods, Evidence, and Study Quality of Health Economic Evaluation Studies for Independently Usable Digital Health Apps: Rapid Review
Abstract
Background: While research on the efficacy of digital health applications (DiHA) is progressing, health economic evaluations (EEs) remain limited but are urgently needed to guide reimbursement and coverage decisions. Existing health policy frameworks frequently overlook cost-effectiveness considerations, and many studies presuppose cost savings without sufficient empirical validation. Although previous reviews have assessed digital health interventions more broadly, none has specifically focused on the cost-effectiveness of those intended for independent patient use.
Objective: This rapid review aims to summarize the current economic evidence and the methods used in health EEs, including modeling practices, and assess the quality of health economic studies on independently usable DiHA for patients.
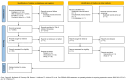
Methods: A systematic search was conducted in 4 electronic databases (PubMed, Cochrane Library, EconBiz, and Web of Science), supplemented by both systematic and unsystematic hand searches. Studies were included on predefined inclusion criteria, considering only complete health EEs of DiHA intended for independent patient use. Data were narratively synthesized. Risk of bias (RoB) was assessed using the Cochrane risk of bias tool 2 (RoB 2), and methodological quality was evaluated using the Consensus on Health Economic Criteria (CHEC) checklist and the Consolidated Health Economic Evaluation Reporting Standards (CHEERS). The review adhered to PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines for implementation and reporting.
Results: A total of 3841 results were identified. After screening the full texts of 82 publications, 7 studies were included in the final analysis. Four of the studies concluded that the app under review was cost-effective compared to the chosen control group. Most of the studies that provided economic evidence incorporated indirect costs and used a societal perspective. All studies used cost-utility analyses (n=7), with the majority based on randomized controlled trials (RCTs) (n=5), considering the health care payer perspective (n=3). Standard care was the most common comparator (n=5). Health outcomes were primarily measured using the EQ-5D (n=3) and condition-specific instruments (n=7). The incremental cost-effectiveness ratio, reported as costs per quality-adjusted life year, was the most frequently reported outcome (n=4). Overall, the quality of the EEs was rated positively using the CHEERS 2022 and CHEC checklists. However, more than half of the underlying RCTs exhibited a high RoB.
Conclusions: DiHA have the potential to be cost-effective, and evaluations of these are of increasing interest. However, health EE is not yet routinely applied in their assessment. Improved reporting of RCT outcomes and greater consistency in modeling practices are needed to support robust EEs in this domain, which could advance evidence-based decision-making and reimbursement policies. This review focused on studies of indication-specific apps, which may have excluded broader applications, highlighting opportunities for more comprehensive research as the field evolves.
Keywords: DiGA; DiHA; cost-effective; cost-effectiveness; digital health; digital health application; digital health intervention; economic evidence; efficacy; health economics; rapid review.
© Valerie Anne Alber, Hendrikje Rödiger, Alessandro Campione, Juliane Schiller, Dominik Burziwoda, Cornelia Henschke. Originally published in the Journal of Medical Internet Research (https://www.jmir.org).
Conflict of interest statement
Figures
References
-
- Institute for Health Metrics and Evaluation (IHME) Global burden of disease 2021: findings from the GBD 2021 study. [30-07-2025];2021 https://www.healthdata.org/sites/default/files/2024-05/GBD_2021_Booklet_... URL. Accessed.
-
- Pankomera R, van Greunen D. A model for implementing sustainable mHealth applications in a resource‐constrained setting: a case of Malawi. E J Info Sys Dev Countries. 2018 Mar;84(2):e12019. doi: 10.1002/isd2.12019. https://onlinelibrary.wiley.com/toc/16814835/84/2 URL. doi. - DOI
-
- Fox G, Connolly R. Mobile health technology adoption across generations: narrowing the digital divide. Information Systems Journal. 2018 Nov;28(6):995–1019. doi: 10.1111/isj.12179. https://onlinelibrary.wiley.com/toc/13652575/28/6 URL. doi. - DOI
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources