Insights from age-stratified endoscopic detection metrics support initiating colorectal cancer screening at age 45
- PMID: 40830845
- PMCID: PMC12362968
- DOI: 10.1186/s12876-025-04213-2
Insights from age-stratified endoscopic detection metrics support initiating colorectal cancer screening at age 45
Abstract
Background and aim: All major U.S. guidelines now validate average-risk colorectal cancer (CRC) screening at 45-49 years of age. We aimed to highlight the importance of promoting colonoscopy among younger populations as part of a comprehensive strategy to reduce the burden of CRC.
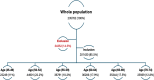
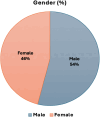
Methods: Our study analyzed data from 235,782 colonoscopy reports of individuals, which were categorized into six age groups: 45-49 years, 50-54 years, 55-59 years, 60-64 years, 65-69 years, and 70-74 years. Parameters such as age, gender, histopathology of polyps, quantity of polyps, and polyp detection rate (PDR) were assessed.
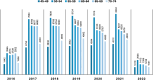
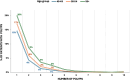
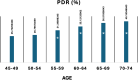
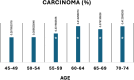
Results: Our study shows a progressive increase in colonoscopy uptake among individuals aged 45-54. PDR increased significantly with age, from 25.7% in the 45-49 group to 40.2% in the 70-74 group (p < 0.05). Notably, the PDR difference between the 45-49 and 50-54 groups was not statistically significant (25.7% vs. 26.8%, p = ns), indicating comparable polyp burden. Carcinoma detection rates followed a similar pattern, with no significant difference between the 45-49 (0.29%) and 50-54 (0.29%) groups, while a substantial rise occurred from age 55 onwards (p < 0.05).
Conclusions: Individuals screened in the 45-49 age group exhibited comparable PDR and carcinoma detection rates to those in the 50-54 age range.
Keywords: Colonoscopy; Colorectal cancer; Colorectal cancer screening; Polyp detection rate (PDR).
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: This study was approved by the Assuta Medical Center Helsinki Ethics Board (Approval Number: 0043-22-ASMC). The requirement for informed consent was waived by the IRB due to the retrospective design of the study and the use of de-identified data in compliance with national regulations and the Declaration of Helsinki. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures

References
-
- Murphy CC, Sandler RS, Sanoff HK, Yang YC, Lund JL, Baron JA. Decrease in incidence of colorectal cancer among individuals 50 years or older after recommendations for Population-based screening. Clin Gastroenterol Hepatology: Official Clin Pract J Am Gastroenterological Association. 2017;15(6):903–e9096. 10.1016/j.cgh.2016.08.037. - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

