Integrated machine learning and population attributable fraction analysis of systemic inflammatory indices for mortality risk prediction in diabetes and prediabetes
- PMID: 40856552
- PMCID: PMC12302434
- DOI: 10.1080/07853890.2025.2536204
Integrated machine learning and population attributable fraction analysis of systemic inflammatory indices for mortality risk prediction in diabetes and prediabetes
Abstract
Background: Chronic systemic inflammation is a key contributor to cardiometabolic complications in diabetes mellitus (DM) and prediabetes (PreDM). Composite inflammatory indices-including neutrophil-to-lymphocyte ratio (NLR), monocyte-to-lymphocyte ratio (MLR), systemic inflammation response index (SIRI), systemic immune-inflammation index (SII), platelet-to-hemoglobin ratio (PHR), and aggregate inflammation systemic index (AISI)-have shown prognostic value for mortality. However, their integrated assessment using machine learning and quantification at the population level remain limited.
Methods: In this retrospective cohort study, 11,304 adults with DM or PreDM from the National Health and Nutrition Examination Survey (NHANES, 2005-2018) were analyzed. The primary outcomes were all-cause and cardiovascular mortality. Associations between inflammatory indices and mortality were evaluated using Cox proportional hazards models. Predictive performance was assessed via Extreme Gradient Boosting (XGBoost), and population attributable fractions (PAFs) estimated the mortality burden related to systemic inflammation.
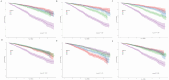
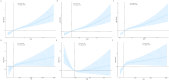
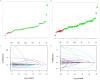
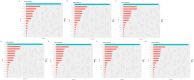
Results: NLR, MLR, SIRI, SII, and AISI were independently associated with all-cause and cardiovascular mortality. MLR showed the strongest association (HR: 2.948 and 3.717 for all-cause and CVD mortality, respectively). XGBoost identified SIRI, SII, AISI, MLR, and NLR as key predictors, with SIRI ranked highest for cardiovascular mortality. Inclusion of inflammatory indices improved model discrimination and calibration. PAF analysis suggested that 10-20% of mortality reduction could be attributed to improved inflammatory profiles.
Conclusion: Systemic inflammatory indices are independent predictors of mortality in individuals with DM or PreDM. Their integration into machine learning models enhances risk prediction and may inform population-level strategies for cardiometabolic risk stratification.
Keywords: Diabetes mellitus; mortality; national health and nutrition examination survey; population attributable fraction; prediabetes; systemic inflammatory indices.
Plain language summary
What is currently known about this topic?Chronic inflammation contributes to the progression of DM or PreDM.Traditional inflammatory markers are costly and less accessible for widespread screenings.Systemic inflammatory indices provide an easily accessible alternative for diagnosis and prognosis.What is the key research question?How does machine learning improve mortality risk prediction, and how does population attributable fraction quantify the contribution of systemic inflammatory indices?What is new?Systemic inflammatory indices are independently associated with mortality in DM or PreDM.Machine learning identifies systemic inflammatory indices as key predictors of mortality.Improving systemic inflammatory indices could reduce mortality events by approximately 10–20%.How might this study influence clinical practice?Integrating systemic inflammatory indices improves risk stratification, and anti-inflammatory strategies may reduce mortality.
Conflict of interest statement
There are no conflicts of interest or competing interests.
Figures


References
-
- Bommer C, Heesemann E, Sagalova V, et al. The global economic burden of diabetes in adults aged 20–79 years: a cost-of-illness study. Lancet Diabet Endocrinol. 2017;5(6):423–430. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
