Passive head-up tilt positioning as an early mobilization strategy in neurocritical care: a prospective-retrospective controlled study
- PMID: 40860977
- PMCID: PMC12370487
- DOI: 10.3389/fneur.2025.1615514
Passive head-up tilt positioning as an early mobilization strategy in neurocritical care: a prospective-retrospective controlled study
Abstract
Background: Early mobilization is recommended in neurocritical care, yet passive mobilization strategies for patients with impaired consciousness remain underexplored. This retrospective matched cohort study, incorporating prospectively collected intervention data, evaluates the clinical efficacy and physiological impact of passive head-up tilt positioning in patients with severe neurological injury.
Methods: We conducted a prospective-retrospective matched cohort study involving 58 patients with traumatic brain injury or hypertensive intracerebral hemorrhage. Twenty-nine patients received standardized passive verticalization using a motorized standing bed; 29 matched controls received standard care. Intracranial dynamics (ICP, CPP, and PRx), respiratory mechanics, intra-abdominal pressure (IAP), and neurological assessments (GCS, CRS-R, ICDSC) were measured at defined intervals. Primary outcomes included NSICU/hospital length of stay, duration of ventilation, complication rates, and long-term functional outcomes.
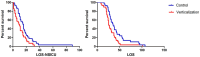
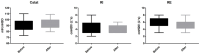
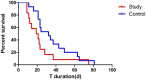
Results: Passive verticalization was well-tolerated and associated with a significant reduction in ICP (10.62 ± 2.13 vs. 8.38 ± 2.27 mmHg, p < 0.05) without affecting CPP or PRx. Neurological function improved significantly (GCS: 7.90 → 10.07; CRS-R: 8.17 → 12.03; all p < 0.05), and delirium severity declined (ICDSC: 5.97 → 1.62). Intervention patients had shorter NSICU and hospital stays, reduced mechanical ventilation duration, earlier enteral nutrition, lower DVT incidence, and superior 6-month ADL and DRS scores.
Conclusion: Passive head-up tilt positioning is a safe, feasible early mobilization strategy in neurocritical care. It improves neurological recovery, reduces complications, and supports long-term functional outcomes. These findings support the incorporation of passive verticalization into early rehabilitation protocols for patients unable to engage in active mobilization.
Keywords: delirium; early mobilization; functional recovery; intracranial pressure; mechanical ventilation; neurocritical care; passive head-up tilt positioning; tilt table therapy.
Copyright © 2025 Jia, Feng, Liu, Yang, Peng and Shao.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


Similar articles
-
Early intervention (mobilization or active exercise) for critically ill adults in the intensive care unit.Cochrane Database Syst Rev. 2018 Mar 27;3(3):CD010754. doi: 10.1002/14651858.CD010754.pub2. Cochrane Database Syst Rev. 2018. PMID: 29582429 Free PMC article.
-
Elevation of the head during intensive care management in people with severe traumatic brain injury.Cochrane Database Syst Rev. 2017 Dec 28;12(12):CD009986. doi: 10.1002/14651858.CD009986.pub2. Cochrane Database Syst Rev. 2017. PMID: 29283434 Free PMC article.
-
Does Augmenting Irradiated Autografts With Free Vascularized Fibula Graft in Patients With Bone Loss From a Malignant Tumor Achieve Union, Function, and Complication Rate Comparably to Patients Without Bone Loss and Augmentation When Reconstructing Intercalary Resections in the Lower Extremity?Clin Orthop Relat Res. 2025 Jun 26;483(9):1680-1695. doi: 10.1097/CORR.0000000000003599. Clin Orthop Relat Res. 2025. PMID: 40569278
-
Repositioning for pressure ulcer prevention in adults.Cochrane Database Syst Rev. 2014 Apr 3;2014(4):CD009958. doi: 10.1002/14651858.CD009958.pub2. Cochrane Database Syst Rev. 2014. Update in: Cochrane Database Syst Rev. 2020 Jun 2;6:CD009958. doi: 10.1002/14651858.CD009958.pub3. PMID: 24700291 Free PMC article. Updated.
-
Nutritional therapy for reducing disability and improving activities of daily living in people after stroke.Cochrane Database Syst Rev. 2024 Aug 15;8(8):CD014852. doi: 10.1002/14651858.CD014852.pub2. Cochrane Database Syst Rev. 2024. PMID: 39145517 Free PMC article.
References
-
- Hemphill JC, 3rd, Greenberg SM, Anderson CS, Becker K, Bendok BR, Cushman M, et al. Guidelines for the Management of Spontaneous Intracerebral Hemorrhage: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. (2015) 46:2032–60. doi: 10.1161/str.0000000000000069, PMID: - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

