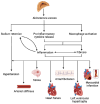
Aldosterone and Cardiovascular Risk Across the Lifespan
- PMID: 40863169
- PMCID: PMC12388298
- DOI: 10.3390/metabo15080553
Aldosterone and Cardiovascular Risk Across the Lifespan
Abstract
Aldosterone excess, particularly in the context of primary aldosteronism, is associated with adverse cardiovascular outcomes. Historically considered a condition of resistant hypertension with hypokalaemia, patients with primary aldosteronism often experienced prolonged diagnostic delay with significant end-organ damage involving the renal, cardiovascular, and central nervous systems at diagnosis. Emerging research has revealed a wide spectrum of renin-independent aldosteronism, ranging from subclinical disease with normal or mildly elevated BP to overt disease marked by resistant hypertension and cardiovascular complications. Subclinical forms of primary aldosteronism have been identified across all age groups, and it is increasingly linked to early signs of adverse cardiac remodelling, even in young adults. Notably, adverse cardiac remodelling was independent of blood pressure. Furthermore, primary aldosteronism confers excess cardiovascular morbidity and mortality compared to blood-pressure-matched essential hypertension. Importantly, these risks can be mitigated through timely diagnosis and treatment with mineralocorticoid receptor antagonists. In this narrative review, we explore the cardiovascular consequences of aldosterone excess, discuss the pathophysiological mechanisms underlying cardiac remodelling, and examine the implications of renin-independent aldosteronism for cardiovascular risk across the lifespan.
Keywords: aldosterone; cardiovascular risk; primary aldosteronism.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
References
-
- Monticone S., D’Ascenzo F., Moretti C., Williams T.A., Veglio F., Gaita F., Mulatero P. Cardiovascular events and target organ damage in primary aldosteronism compared with essential hypertension: A systematic review and meta-analysis. Lancet Diabetes Endocrinol. 2018;6:41–50. doi: 10.1016/S2213-8587(17)30319-4. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources