Interstitial lung disease epidemiology and etiology in patients with solid malignant tumors: a systematic literature review
- PMID: 40890043
- PMCID: PMC12490398
- DOI: 10.1080/14796694.2025.2550928
Interstitial lung disease epidemiology and etiology in patients with solid malignant tumors: a systematic literature review
Abstract
Background: Interstitial lung disease (ILD) can occur in patients with cancer. ILD can be caused by anti-cancer treatments (drug-induced [DI] ILD), but also by opportunistic infection, and non-drug-related etiologies. This systematic literature review (SLR) investigated the epidemiology and etiology of non-DI ILD and DI ILD management and outcomes in patients with solid cancers.
Methods: Databases were searched to August 2023 using terms for ILD and solid cancers. Relevant congresses held 2021-2023 and SLR bibliographies were hand-searched. Records were screened by two independent reviewers. Inclusion criteria comprised ILD epidemiology outcomes, ILD clinical management, and survival outcomes.
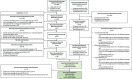
Results: Of 4,519 unique records screened, 55 full texts were included (six from supplementary sources) and 37 were prioritized for extraction. Studies were frequently retrospective cohort studies in Japan (n = 21). Patients mostly had lung cancers (n = 32) and received immune checkpoint inhibitors (n = 24). Reporting of non-DI ILD was limited and associated with radiation therapy (n = 4) or surgery (n = 1). Most studies reported DI ILD outcomes only (n = 31).
Conclusion: The limited evidence of non-DI ILD indicates that prompt intervention to manage ILD until other ILD etiologies have been ruled out remains key to preventing progression of both cancer and ILD.Protocol registration http://www.crd.york.ac.uk/prospero identifier: CRD42023463573.
Keywords: cancer; epidemiology; epidemiologyInterstitial lung disease; etiology; solid malignancy.
Plain language summary
Interstitial lung disease, or “ILD,” is a group of conditions that cause scarring and swelling in the lungs. This makes it harder to breathe and get enough oxygen. New cancer drugs can work well to treat a person’s cancer, but they can sometimes cause ILD as a side-effect (known as “drug-induced” ILD). ILD can have other causes unrelated to cancer treatment. For example, some lung infections can cause ILD. When ILD occurs, a person’s cancer treatment has to be paused until the lung condition improves, which could worsen outcomes.We aimed to find out how commonly these other causes of ILD occur in people with solid cancers (cancers that affect tissues and organs such as breast, lung, and liver) and what these causes are. We also looked at survival outcomes in patients who develop ILD and how ILD is treated.We identified 55 published studies, mostly from Japan and in people with lung cancer. ILD not caused by cancer treatment was rarely reported and was linked to radiation therapy or surgery in all of the studies that we reviewed. No cases of ILD caused by infection were found in these studies, even though some known cases have been reported in medical case reports. We found that people had shorter survival times on average if they had severe ILD or if the ILD developed soon after starting cancer treatment.Although we did not find many studies reporting other causes of ILD in people with cancer, it is still very important that doctors follow guidelines closely to find out whether the ILD has been caused by a person’s cancer treatment or by something else. While doing so, doctors should treat both possible causes until infection can be ruled out.As new cancer treatments that can cause ILD are used more and more widely, doctors need to understand ILD and its different potential causes. Finding out what has caused the ILD is important so that it can be treated appropriately and promptly, and the person can restart cancer treatment once the condition has improved.
Conflict of interest statement
Medical writing and editorial assistance were provided by Oliver Palmer (Costello Medical, UK) and was funded by AstraZeneca, based on the authors’ input and direction, and in accordance with Good Publication Practice (GPP 2022).
Figures
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical