Efficacy, Effectiveness, and Safety of Phenobarbital in the Treatment of Cholestasis and as a Premedication to Improve Diagnostic Accuracy of Hepatobiliary Scintigraphy: A Systematic Review
- PMID: 40894347
- PMCID: PMC12391896
- DOI: 10.47895/amp.vi0.10948
Efficacy, Effectiveness, and Safety of Phenobarbital in the Treatment of Cholestasis and as a Premedication to Improve Diagnostic Accuracy of Hepatobiliary Scintigraphy: A Systematic Review
Abstract
Objective: Phenobarbital is an inductor of microsomal hepatic enzyme and used as choleretic for cholestatic liver disease to enhance bile flow. It is also used as a premedication for hepatobiliary scintigraphy (HIDA) scan to improve diagnostic accuracy for an obstructive liver disease. We reviewed the available literature on the use of Phenobarbital for treatment of cholestasis and its utility as a premedication for HIDA scan.
Methods: All published studies before June 30, 2023 that investigated the efficacy, effectiveness or safety of Phenobarbital in cholestatic jaundice and its effect on the accuracy of hepatobiliary scintigraphy in diagnosis of obstructive jaundice were included. Electronic databases were searched including MEDLINE via PubMed,Cochrane Library, medRxIV, BioRxIV, as well as the following registries for ongoing and completed trials: ClinicalTrials.gov (USA); ChiCTR.org. (China); and the WHO International Clinical Trials Registry Platform. We screened abstracts, reviewed full texts, and extracted relevant information on study design, settings, population, and outcomes. There was no age and language restriction. Two reviewers independently rated the quality of included studies using: Joanna Briggs Institute critical appraisal tool for case reports, case series, and diagnostic accuracy; Newcastle - Ottawa Quality Assessment Scale for cohort studies, and Cochrane Risk of Bias for Randomized Trials. Risk of bias was appraised and GRADE certainty of evidence was judged. Pooled analysis was done using Stata 14 and reported as sensitivity and specificity.
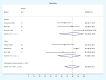
Results: Included were nine reports on Phenobarbital as treatment for cholestasis (one case report, five case series, one cohort and two randomized studies) and seven studies (four diagnostics, two cohorts, one randomized trial) on its use as a premedication for HIDA scan. The quality of case report and case series were considered fair; cohort studies as good; and diagnostic studies were included based on overall assessment. The randomized studies had some or high risk for bias due to concerns in randomization process, measurement of outcome, and risk in the selection of reported results.There were 31 patients (16 adults and 15 children) from case reports and case series. Of the 16 adults, serum total bilirubin concentrations declined from 4 to 70% from baseline in 13 of 15 (87%) patients after Phenobarbital was given at 120 to 250 mg per day from 22 days to five months. Eleven of 14 with pruritus at onset also had improvement in intensity of itching. Of the 15 pediatric patients, ten (67%) showed a decrease from 10 to 60% of the baseline total bilirubin but not a normalization with Phenobarbital intake at a dose of 3 to 12 mg/kg/day from one to 21 months. Five of 14 children also had relief of itching after treatment.Phenobarbital compared to Ursodeoxycholic acid had limited efficacy in reducing the bilirubin levels in neonates and young infants with cholestasis.Moderate certainty evidence showed that with Phenobarbital pretreatment, the hepatobiliary scan done on patients with neonatal cholestasis had 100% (CI 99.2, 100; I2 = 0.0%) sensitivity and 80.2% (CI 65.4, 92.1; I2 = 76.6%) specificity while no Phenobarbital pretreatment had 100% (94.9, 100; I2 = 0.0%) sensitivity and 89.5% (CI 77.0, 98.1; I2 = 11.4%) specificity. Adverse effects of Phenobarbital were drowsiness, lethargy, poor feeding, and irritability.
Conclusion: There was limited effectiveness of Phenobarbital in decreasing bilirubin levels in cholestatic liver disease. Moderate certainty evidence demonstrated that premedication with Phenobarbital did not improve the specificity of HIDA scan in the diagnosis of obstructive jaundice of infancy. Neurologic symptoms were observed with Phenobarbital intake.
Keywords: cholestasis; phenobarbital; pruritus; scintigraphy.
© The Author(s) 2025.
Conflict of interest statement
All authors declared no conflicts of interest.
Figures






References
-
- Vitug J, Avila J, Gregorio G. Histological pattern and outcome of Filipino children with liver disease who underwent percutaneous liver biopsy: a five year survey. Acta Med Philipp. 2015. Dec; 49(4):12–7. doi: 10.47895/amp.v49i4.886. - DOI
-
- Costa S, Barone G, Catenazzi P, Romagnoli C. Parenteral nutrition associated cholestasis. Ital J Pediatr. 2015. Sep 24;41(Suppl 1):A4. doi: 10.1186/1824-7288-41-S1-A4. PMCID: . - DOI
LinkOut - more resources
Full Text Sources
