The epidemiology, clinical burden, and prevention of intrauterine adhesions (IUAs) related to surgically induced endometrial trauma: a systematic literature review and selective meta-analyses
- PMID: 40914965
- PMCID: PMC12584913
- DOI: 10.1093/humupd/dmaf019
The epidemiology, clinical burden, and prevention of intrauterine adhesions (IUAs) related to surgically induced endometrial trauma: a systematic literature review and selective meta-analyses
Abstract
Background: Reproductive-age women with intrauterine adhesions (IUAs) following uterine surgery may be asymptomatic or may experience light or absent menstruation, infertility, preterm delivery, and/or peripartum hemorrhage. Understanding procedure- and technique-specific risks and the available evidence on the impact of surgical adjuvants is essential to the design of future research.
Objective and rationale: While many systematic reviews have been published, most deal with singular aspects of the problem. Consequently, a broadly scoped systematic review and selective meta-analyses identifying evidence strengths and gaps are necessary to inform future research and treatment strategies.
Search methods: A systematic literature review was performed seeking evidence on IUA incidence following selected uterine procedures and the effectiveness of hysteroscopic adhesiolysis on menstrual, endometrial, fertility, and pregnancy-related outcomes. An evaluation of the impact of surgical adjuvants designed to facilitate adhesion-free endometrial repair was included. Searches were conducted in the PubMed, Embase, and Cochrane databases following PRISMA guidelines and included English-language publications from inception to 8 November 2024. Inclusion criteria restricted articles to those reporting IUA epidemiology or related clinical outcomes. Risk of bias assessment used the US NIH tools for interventional and observational studies. Meta-analyses were conducted and reported only for outcomes where there were sufficient data. Per analysis, we report on proportions (with 95% CI), heterogeneity (I2), and the risk of bias for each study included.
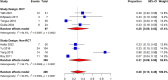
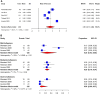
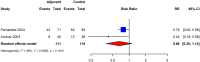
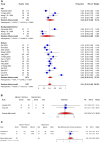
Outcomes: The review identified 249 appropriate publications. The risks of new-onset IUAs following the removal of products of conception after early pregnancy loss, hysteroscopic myomectomy, and hysteroscopic metroplasty for septum correction were 17% (95% CI: 11-25%; 13 studies, I2 = 87%, poor to good evidence quality), 16% (95% CI: 6-28%; 8 studies, I2 = 93%, fair to good evidence quality), and 28% (95% CI: 13-46%; 8 studies, I2 = 91%, fair to good evidence quality), respectively. For primary IUA prevention with adjuvant intrauterine gel barriers, the relative risks were 0.45 (95% CI: 0.30-0.68; three studies, I2 = 0%, poor to good evidence quality), 0.38 (95% CI: 0.20-0.73; three studies, I2 = 0%, fair evidence quality), and 0.29 (95% CI: 0.12-0.69; three studies, I2 = 0%, fair to good evidence quality), respectively, following the above potentially adhesiogenic procedures. Following adhesiolysis without adjuvants, the IUA recurrence rate was 35% (95% CI: 24-46%; 13 studies, I2 = 95%, poor to good evidence quality), similar to the rate of 43% for both those treated adjuvantly with an intrauterine balloon (95% CI: 35-51%; 14 studies, I2 = 85%, poor to good evidence quality), or an IUD (95% CI: 27-59%; four studies, I2 = 85%, fair to good evidence quality). The recurrence rate for secondary prevention with gel barriers was 28% (95% CI: 4-62%; three studies, I2 = 94%, good evidence quality). Notably, there was an excess rate of associated adverse obstetrical outcomes, including preterm delivery, placenta accreta spectrum, placenta previa, peripartum hemorrhage, and hysterectomy, with evidence demonstrating the beneficial impact of adjuvant therapies on these outcomes.
Wider implications: This systematic review comprehensively analyzes IUA formation following uterine surgical procedures and adjuvant therapy effectiveness. Even following adhesiolysis, it is apparent that the basilar endometrial trauma thought to facilitate the formation of IUAs may persist and contribute to adverse reproductive outcomes. Many critical gaps remain in our knowledge of the pathogenesis, prevention, and management of endometrial trauma and IUAs.
Pregistration number: PROSPERO (ID: CRD42023366218).
Keywords: endometrial trauma; hysteroscopy; infertility; intrauterine adhesions; metroplasty; myomectomy; placenta accreta spectrum; postpartum hemorrhage; retained products of conception; septum removal.
© The Author(s) 2025. Published by Oxford University Press on behalf of European Society of Human Reproduction and Embryology.
Conflict of interest statement
Axtria Inc., a consulting company, received consultancy fees from Rejoni Inc., and includes D.S., A.K.J., R.G., J.K., and C.M. A.B.H. has received honoraria for a presentation from Merck and contributions to travel expenses from Merck and Nordic Pharma, as well as participates in a data safety monitoring board for Womed. C.A.S. has an academic research connection with Rejoni Inc., as she is the study site Principal Investigator at the University of Texas at Austin for Rejoni Inc. for a randomized clinical trial investigating IUAs with intrauterine gel placement, titled ‘Safety and Effectiveness of Juveena’, although she does not receive direct funding from Rejoni Inc. C.A.S. also declares consulting fees from Womed for expert hysteroscopist reviewing of video recordings for the PREG2 study. M.G.M. received payments to his consulting company from Rejoni Inc. and Womed and he is the Founder and Chair of WHrC, a not-for-profit research and advocacy organization. B.B. has an academic research connection with Rejoni Inc. as he is a study site Principal Investigator at the University of Wisconsin-Madison for a randomized clinical trial of intrauterine gel to prevent IUAs (Safety and Effectiveness of Juveena), although he did not receive direct funding from Rejoni. Due to his role as an inventor, M.H.E. has received royalties for the international sales of Truclear by Medtronic, Minneapolis MN, USA and MyoSure by Hologic, San Diego CA, USA until November 2022 and received up to date royalties for the sales of ExEm Foam in the USA by IQ Medical Ventures BV, Rotterdam, the Netherlands. He has also received honoraria for educational events related to ExEm Foam from Gedeon-Richter, Budapest, Hungary. H.G.H. has a research contract with May Health and Rejoni Inc. and also has received royalties from UpToDate®. She has also received consulting fees from Amazon/Emblem Health as she is a Medical Advisory Board Member, as well as a member of Allara Health, where she is a Scientific Advisor. Furthermore, H.G.H. has received speaker honoraria from the Endocrine Society, is a board member of Comet Study/PI Anuja Dokras, is the Secretary/Treasurer for Society of Reproductive Endocrinology, and has received stock options from Allara Health.
Figures












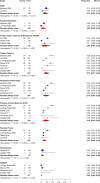


References
-
- Aboulghar MM, Shoeir IK, Momtaz M, El Mohammady M, Ezzat H. A comparative study of 2-dimensional sonohysterography versus 3-dimensional sonohysterography in infertile patints with utrine cavity lesions and abnormalitiies. Middle East Fertil Soc J 2011;16:67–71.
-
- Acunzo G, Guida M, Pellicano M, Tommaselli GA, Di Spiezio Sardo A, Bifulco G, Cirillo D, Taylor A, Nappi C. Effectiveness of auto-cross-linked hyaluronic acid gel in the prevention of intrauterine adhesions after hysteroscopic adhesiolysis: a prospective, randomized, controlled study. Hum Reprod 2003;18:1918–1921. - PubMed
-
- Ajjammanavar V, , HiremathND, , Jayashree S. Role of hysterolaparoscopy in infertility. International Journal of Infertility and Fetal Medicine 2020;11:5–10. 10.5005/jp-journals-10016-1196. - DOI
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

