Salvage Surgery: A Concrete Opportunity in Unresectable Non-Small Cell Lung Cancer Following Definitive Chemo-Immunotherapy
- PMID: 41008811
- PMCID: PMC12468883
- DOI: 10.3390/cancers17182967
Salvage Surgery: A Concrete Opportunity in Unresectable Non-Small Cell Lung Cancer Following Definitive Chemo-Immunotherapy
Abstract
Background: The advent of immunotherapy has significantly improved survival outcomes in advanced non-small cell lung cancer (NSCLC). In this evolving context, salvage surgery has emerged as a potential curative strategy, despite the risk of serious complications. This study aimed to evaluate the safety and efficacy of surgical resection following chemo-immunotherapy in patients with initially unresectable NSCLC.
Methods: We retrospectively analyzed patients with stage III-IVB NSCLC who underwent salvage surgery at our institution between January 2019 and June 2024. All cases were initially deemed unresectable by a multidisciplinary tumor board. Perioperative complications, complete (R0) resection rate, major pathologic response (MPR), complete pathologic response (pCR), progression-free survival (PFS), and overall survival (OS) were analyzed.
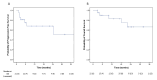
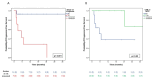
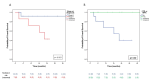
Results: Twenty-one patients (thirteen males, eight females; median age: 68 years [IQR: 9]) were included. Reasons for initial unresectability were metastatic disease (28.6%), N2 bulky disease (14.3%), local invasiveness (33.3%), or a combination of factors (23.7%). Chemo-immunotherapy was administered in 19 patients (90.5%), while 2 (9.5%) received immunotherapy alone, with a median of four treatment cycles (IQR: 1). Complete (R0) resection was achieved in all patients (100%). Anatomical resections were performed in 17 patients (81%), predominantly lobectomies (66.7%). There were no intraoperative or major postoperative complications, and 30-day mortality was zero. Median hospital stay was 7 days (IQR: 4). pCR and MPR were achieved in 33.3% and 14.3% of patients, respectively. After a median follow-up of 17 months (IQR: 19), the estimated 3-year PFS and OS were 50.9% and 66.3%, respectively. Recurrences included locoregional (4.8%), distant (14.3%), and combined (14.3%). Cox regression analysis identified stage III at diagnosis (OR: 0.292; 95% CI: 0.093-0.912; p = 0.034) and achieved pCR or MPR (OR: 0.113; 95% CI: 0.013-0.959; p = 0.046) as independent predictors of improved PFS.
Conclusions: Salvage surgery after chemo-immunotherapy in initially unresectable NSCLC appears to be a safe and effective strategy in selected patients, offering favorable pathological responses and encouraging mid-term oncologic outcomes.
Keywords: chemo-immunotherapy; complete pathologic response; immune checkpoint inhibitors; major pathologic response; neoadjuvant therapy; non-small cell lung cancer; salvage surgery.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
References
-
- Gray J.E., Villegas A., Daniel D., Vicente D., Murakami S., Hui R., Kurata T., Chiappori A., Lee K.H., Cho B.C., et al. Three-year overall survival with durvalumab after chemoradiotherapy in stage III NSCLC-update from PACIFIC. J. Thorac. Oncol. 2020;15:288–293. doi: 10.1016/j.jtho.2019.10.002. - DOI - PMC - PubMed
-
- Bott M., Cools-Lartigue J., See Tan K., Dycoco J., Bains M.S., Downey R.J., Huang J., Isbell J.M., Molena D., Park B.J., et al. Safety and feasibility of lung resection after immunotherapy for metastatic or unresectable tumors. Ann. Thorac. Surg. 2018;106:178–183. doi: 10.1016/j.athoracsur.2018.02.030. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources

