Clinical management and burden of cytomegalovirus in D+/R-Kidney transplant recipients in Canada
- PMID: 41050692
- PMCID: PMC12488418
- DOI: 10.3389/fimmu.2025.1618748
Clinical management and burden of cytomegalovirus in D+/R-Kidney transplant recipients in Canada
Erratum in
-
Correction: Clinical management and burden of cytomegalovirus in D+/R-Kidney transplant recipients in Canada.Front Immunol. 2025 Oct 14;16:1712602. doi: 10.3389/fimmu.2025.1712602. eCollection 2025. Front Immunol. 2025. PMID: 41164197 Free PMC article.
Abstract
Purpose: To document prophylactic practices, infection patterns, and disease burden to inform strategies for CMV management in high-risk kidney transplant recipients.
Methods: A retrospective cohort of 311 consecutive CMV D+/R- kidney recipients were enrolled from 7 Canadian programs over 4 years (2018-2021) to provide data on demographic, clinical, therapeutic and health resource use during the 1st year post-transplant.
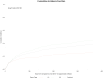
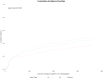
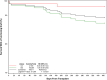
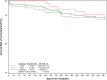
Results: Themedian age was 58 (46, 67) years, 69% were male, and 53% were White. Diabetes was the principal cause of kidney failure (19%). 208 (69%) received a deceased donor graft; 76 (24%) had ATG induction, and 84% had maintenance therapy with tacrolimus and MMF/MPA ± prednisone. All received antiviral prophylaxis, 90% with valganciclovir, for a median of 180 days. 106 (34%) developed CMV viremia (median peak viral load 14,224 IU/ml) at a median of 218 days, of whom 46 (43%) had CMV disease and 15 (14%) had recurrent infection. Myelotoxicity occurred in 121 (39%) patients at a median of 88 days, lasting a median of 30 days. Opportunistic infections occurred in 119 patients (38%) at a median of 53 days. 141 patients (45%) were hospitalized, 50 (16%) more than once. 20 patients (6%) had biopsy-confirmed rejection, and 293 (94%) were alive with a functioning graft at 1 year.
Conclusion: Current prophylaxis strategies fail to prevent CMV infection in 34% of high-risk patients. Myelotoxicity, opportunistic infection, reduced immunosuppression, and hospitalization remain common and serious complications. More effective and less toxic personalized treatment strategies are required to minimize these risks and burdens.
Keywords: antiviral prophylaxis and treatment; cytomegalovirus; graft failure; hospitalization; immunosuppression; kidney transplantation; leukopenia; superinfection.
Copyright © 2025 Gill, House, Chagla, Tchervenkov, Kim, Vinson, Cervera, Keown, Sun, Khoury and Ghakis.
Conflict of interest statement
PK is a Director of Syreon Corporation which conducted the study on behalf of Merck Canada Inc. and the investigators. SS, CK and CG were employees of Merck Canada Inc. at the time of the trial/study and may hold stock in the company. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


References
-
- Cowan J, Bennett A, Fergusson N, McLean C, Mallick R, Cameron DW, et al. Incidence rate of post-kidney transplant infection: A retrospective cohort study examining infection rates at a large Canadian multicenter tertiary-care facility. Can J Kidney Health Dis. (2018) 5:2054358118799692. doi: 10.1177/2054358118799692, PMID: - DOI - PMC - PubMed
-
- Leeaphorn N, Garg N, Thamcharoen N, Khankin EV, Cardarelli F, Pavlakis M. Cytomegalovirus mismatch still negatively affects patient and graft survival in the era of routine prophylactic and preemptive therapy: A paired kidney analysis. Am J Transpl. (2019) 19:573–84. doi: 10.1111/ajt.15183, PMID: - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

