Metabolomic profiling of patients with lupus nephritis reveals unique metabolites that are modulated through type I interferon inhibition by anifrolumab treatment in a phase 2 trial
- PMID: 41052889
- PMCID: PMC12506476
- DOI: 10.1136/rmdopen-2025-005932
Metabolomic profiling of patients with lupus nephritis reveals unique metabolites that are modulated through type I interferon inhibition by anifrolumab treatment in a phase 2 trial
Abstract
Objective: Patients with systemic lupus erythematosus (SLE) commonly develop lupus nephritis (LN), the most frequent severe organ manifestation of this systemic autoimmune disease. Using serum and urine samples from a phase 2 trial in LN, we investigated that how the LN metabolome is modulated in response to type I interferon receptor blockade with anifrolumab, an approved treatment for moderate to severe SLE.
Methods: Patients in TULIP-LN (NCT02547922) received standard therapy plus intravenous anifrolumab or placebo. Untargeted metabolomics analysis was performed on serum and urine samples from 128 and 119 patients, respectively. Metabolites impacted by anifrolumab and their associations with clinical, serological and kidney measures of LN disease activity were examined. An in vitro model was used to validate the impact of anifrolumab on metabolite-induced inflammation.
Results: In serum, indoxyl sulfate (IS) and cytosine were the metabolites most modulated by anifrolumab, while baseline levels correlated with measures of kidney damage. In urine, uracil and cytosine were the most modulated by anifrolumab and levels of these metabolites were associated with serological markers of disease activity. Anifrolumab reduced markers of vascular dysfunction and inflammation upregulated by IS in in vitro models. Baseline urine uracil levels predicted response to anifrolumab intensive regimen at Week 52.
Conclusion: Our findings establish a connection between type I interferon signalling, pyrimidine metabolism and uremic toxins in patients with LN and support the evaluation of urine uracil as a potential biomarker of response to anifrolumab.
Keywords: Autoimmune Diseases; Biological Therapy; Lupus Nephritis.
© Author(s) (or their employer(s)) 2025. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ Group.
Conflict of interest statement
Competing interests: DJ: Consultant: Amgen, Astra-Zeneca, CSL Vifor, GSK, Novartis, Roche and Takeda; Speaker's bureau: AMGEN, CSL Vifor and Otsuka; and Grant/research support: CSL Vifor, GSK and Roche; EM: Advisor/review panel member: AbbVie, AstraZeneca, Janssen and Pfizer; Consultant: AbbVie, GSK, Hi Bio, Alpine Immunology and Pfizer; Speaker/honoraria: AbbVie, Amgen, AstraZeneca, Janssen, Lilly, Pfizer, Sanofi and Sandoz; and Grant/research support: AstraZeneca, Bristol Myers Squibb, GSK, Janssen, Lilly, Novartis and Roch; ZA: Advisor/review panel member: AstraZeneca, GSK and Novartis; Speaker/honoraria: AstraZeneca and GSK; and Grant/research support: Amgen, AstraZeneca, GSK, Novartis and Roche; PGG, DM, CA, HS, AS, KW and HA-M: Employees of AstraZeneca; ELA, CDP, XT, SH, EC, PZB, AP, CL and NF: Employees and hold intellectual property/patents, stock options or bond holdings: AstraZeneca.
Figures
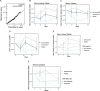




References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
