Predicting arrhythmia recurrence post-ablation in atrial fibrillation using explainable machine learning
- PMID: 41087542
- PMCID: PMC12521406
- DOI: 10.1038/s43856-025-01058-4
Predicting arrhythmia recurrence post-ablation in atrial fibrillation using explainable machine learning
Abstract
Background: Following atrial fibrillation ablation, it is challenging to distinguish patients who will remain arrhythmia-free from those at risk for recurrence. New explainable machine learning (xML) techniques allow for systematic assessment of arrhythmia recurrence risk following catheter ablation. We aim to develop an xML algorithm that predicts recurrence and reveals key risk factors to facilitate better follow-up strategy after an ablation procedure.
Methods: We reconstructed pre-and post-ablation models of the left atrium (LA) from late gadolinium enhanced magnetic resonance (LGE-MRI) for 67 patients. Patient-specific features (LGE-based measurements of pre/post-ablation arrhythmogenic substrate, LA geometry metrics, computational simulation results, and clinical risk factors) trained a random forest classifier to predict recurrent arrhythmia. We calculated each risk factor's marginal contribution to model decision making via SHapley Additive exPlanations (SHAP).
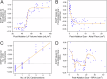
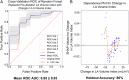
Results: The classifier accurately predicts post-ablation arrhythmia recurrence (mean receiver operating characteristic [ROC] area under the curve [AUC]: 0.80 ± 0.04; mean precision-recall [PR] AUC: 0.82 ± 0.08). SHAP analysis reveals that of 89 features tested, the key population risk factors for recurrence are: large left atrium, low LGE-quantified post-ablation scar in the atrial floor region, and previous attempts at direct current cardioversion. We also examine patient-specific recurrence predictions, since xML allows us to understand why a particular individual can have large prediction weights for some categories without tipping the balance towards an incorrect prediction. Finally, we validate our model in a completely new, 15-patient retrospective holdout cohort (80% correct).
Conclusion: Our SHAP-based explainable machine learning approach is a proof-of-concept clinical tool to explain arrhythmia recurrence risk in patients who underwent ablation by combining patient-specific clinical profiles and LGE-derived data.
Plain language summary
Atrial fibrillation (AFib) is a common heart rhythm problem. It is treated by catheter ablation, in which a thin flexible tube is inserted into the heart and a treatment administered that will destroy the part of the heart from which the abnormal heart rhythms originate. We used a computational method to predict whether AFib would come back after ablation. We trained our model on detailed heart scans, clinical data, and computer simulations from 67 patients. Our method accurately predicted which patients would have a recurrence and highlighted important risk factors, such as large heart size, specific scar distributions after ablation, and people having had previous electrical shock therapy. We confirmed our model worked well in a separate group of 15 patients. Our approach could help doctors better understand individual patient risks and plan more effective follow-up care after ablation.
© 2025. The Author(s).
Conflict of interest statement
Competing interests: The authors declare no competing interests.
Figures





References
-
- Andrade, J., Khairy, P., Dobrev, D. & Nattel, S. The clinical profile and pathophysiology of atrial fibrillation: relationships among clinical features, epidemiology, and mechanisms. Circ. Res.114, 1453–1468 (2014). - PubMed
-
- Kobza, R. et al. Late recurrent arrhythmias after ablation of atrial fibrillation: incidence, mechanisms, and treatment. Heart Rhythm1, 676–683 (2004). - PubMed
-
- Vizzardi, E. et al. Risk factors for atrial fibrillation recurrence: a literature review. J. Cardiovasc. Med.15, 235–253 (2014). - PubMed
-
- Santoro, F. et al. Impact of uncontrolled hypertension on atrial fibrillation ablation outcome. JACC Clin. Electrophysiol.1, 164–173 (2015). - PubMed
-
- Wang, T. J. et al. Obesity and the risk of new-onset atrial fibrillation. JAMA292, 2471–2477 (2004). - PubMed
Grants and funding
- R01 HL158668/HL/NHLBI NIH HHS/United States
- T32 EB001650/EB/NIBIB NIH HHS/United States
- R01HL158668/U.S. Department of Health & Human Services | NIH | National Heart, Lung, and Blood Institute (NHLBI)
- T32EB001650/U.S. Department of Health & Human Services | NIH | National Institute of Biomedical Imaging and Bioengineering (NIBIB)
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

