Respiratory System Compliance Predicts Outcome After Lung Transplantation-A Retrospective Single Center Study
- PMID: 41096021
- PMCID: PMC12525188
- DOI: 10.3390/jcm14196941
Respiratory System Compliance Predicts Outcome After Lung Transplantation-A Retrospective Single Center Study
Abstract
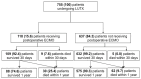
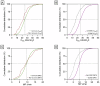
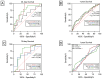
Background: Outcome prediction in patients undergoing lung transplantation (LUTX) for end-stage pulmonary disease can be challenging. We examined the prognostic value for mortality of respiratory system compliance (CRS) and mechanical power of ventilation (MP) at end of surgery in patients undergoing LUTX for end-stage pulmonary disease. Methods: In this single-center retrospective study, we included 755 patients undergoing LUTX between 2014 and 2023. The primary endpoint of this study was 1-year mortality, with 30-day mortality serving as a secondary endpoint. We conducted both univariate and multivariate analyses and constructed Receiver Operating Characteristic curves. Results: Of 755 patients, 1.9% and 12.2% patients died within 30 days and 1 year after LUTX. Fifteen-point four percent of all patients required extracorporeal membrane oxygenation (ECMO) prolongation into the early postoperative period. CRS, but not MP was higher in 1-year survivors compared to non-survivors [median 25.8 mL/cmH2O (20.1, 32.1) and 22.5 mL/cmH2O (15.2, 28.4); p < 0.001] and [median 10.0 J/min (7.8, 12.0) and 9.3 J/min (6.2, 13.1); p = 0.329]. Moreover, low CRS < 25.1 mL/cmH2O remained an independent factor for increased 1-year mortality after LUTX. Additionally, increased MP and CRS were predictive for 30-day survival with an acceptable area under the curve of 0.758 (95% CI: 0.6-0.8; p < 0.001) and 0.735 (95% CI: 0.5-0.9; p = 0.003), and a sensitivity and specificity of 51% and 75.5% for MP and 50% and 85% for CRS, respectively. Conclusions: Postoperative CRS serves as a significant independent predictor for short and long-term outcome in patients undergoing LUTX with and without ECMO prolongation into the early postoperative period.
Keywords: lung transplantation; mechanical power; outcome; respiratory system compliance.
Conflict of interest statement
All authors declare that they have no competing interests.
Figures
References
-
- Raskin J., Vanstapel A., Verbeken E.K., Beeckmans H., Vanaudenaerde B.M., Verleden S.E., Neyrinck A.P., Ceulemans L.J., Van Raemdonck D.E., Verleden G.M., et al. Mortality after lung transplantation: A single-centre cohort analysis. Transpl. Int. 2020;33:130–141. doi: 10.1111/tri.13540. - DOI - PubMed
-
- Veraar C., Kirschner E., Schwarz S., Jaksch P., Hoetzenecker K., Tschernko E., Dworschak M., Ankersmit H.J., Moser B. Follistatin-like 1 and Biomarkers of Neutrophil Activation Are Associated with Poor Short-Term Outcome after Lung Transplantation on VA-ECMO. Biology. 2022;11:1475. doi: 10.3390/biology11101475. - DOI - PMC - PubMed
-
- Veraar C., Schwarz S., Thanner J., Direder M., Boehm P.M., Harnoncourt L., Ortmayr J., Veraar C., Mascherbauer J., Klepetko W., et al. Transient perioperative inflammation following lung transplantation and major thoracic surgery with elective extracorporeal support: A prospective observational study. Ann. Transl. Med. 2021;9:385. doi: 10.21037/atm-20-4771. - DOI - PMC - PubMed
-
- Snell G.I., Yusen R.D., Weill D., Strueber M., Garrity E., Reed A., Pelaez A., Whelan T.P., Perch M., Bag R., et al. Report of the ISHLT Working Group on Primary Lung Graft Dysfunction, part I: Definition and grading—A 2016 Consensus Group statement of the International Society for Heart and Lung Transplantation. J. Heart Lung Transplant. 2017;36:1097–1103. doi: 10.1016/j.healun.2017.07.021. - DOI - PubMed
LinkOut - more resources
Full Text Sources

