Efficacy of different psychological interventions for the treatment of inflammatory bowel disease: a systematic review and network meta-analysis
- PMID: 41127398
- PMCID: PMC12537889
- DOI: 10.3389/fmed.2025.1630034
Efficacy of different psychological interventions for the treatment of inflammatory bowel disease: a systematic review and network meta-analysis
Abstract
Objective: National guidelines for inflammatory bowel disease (IBD) recommend psychotherapy, but the relative efficacy of different psychological interventions is unclear. To address this issue, we conducted a systematic review and network meta-analysis.
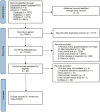
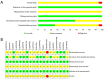
Methods: The PubMed, Cochrane Library, Embase, and Web of Science databases were systematically searched for randomized controlled trials (RCTs) from the databases' inception to October 11, 2024. The primary outcomes were depression, anxiety, and stress levels, and the secondary outcomes were disease activity and quality of life. Two reviewers independently selected studies, extracted data according to pre-specified criteria, and assessed the risk of bias using the Cochrane Collaboration's risk of bias tool. Network meta-analysis was performed using Stata 16.0 and R. Comparators included usual care (UC), waiting list (WL), and head-to-head comparisons between psychological interventions.
Results: Nineteen RCTs (1,637 participants) evaluating 12 interventions were included. Compared with WL, mindfulness interventions (MI) (SMD -0.63, 95% CI -1.20 to -0.05) and cognitive behavioral therapy (CBT) (SMD -0.54, 95% CI -0.90 to -0.17) reduced depression. Compared with WL, acceptance and commitment therapy with a compassion-focused group component (SMD -1.15, 95% CI -2.21 to -0.05), acceptance and commitment therapy (SMD -1.01, 95% CI -1.83 to -0.16), and CBT (SMD -0.75, 95% CI -1.41 to -0.09) reduced anxiety. For QoL, MI improved outcomes versus WL (SMD 2.21, 95% CI 0.25-4.12) and versus UC (SMD 1.82, 95% CI 0.53-3.10). No significant differences were detected for stress or disease activity versus WL or UC (where available). SUCRA rankings suggested that MI ranked highest for depression and QoL, compassion-focused ACT ranked highest for anxiety and disease activity, and CBT ranked highest for stress.
Conclusion: Psychological interventions appear to provide adjunctive benefits for people with IBD. MI shows consistent advantages for depression and QoL; ACT (with or without a compassion-focused component) and CBT reduce anxiety; CBT ranks favorably for stress. Effects on disease activity remain uncertain, and further high-quality trials are warranted.
Systematic review registration: https://www.crd.york.ac.uk/PROSPERO/view/CRD4202460005.
Keywords: depression; inflammatory bowel disease; network meta-analysis; psychotherapy; quality of life.
Copyright © 2025 Wang, Ding, Liu, Sun, Zhang, Xiao, Cai and Lin.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures



References
-
- Wang R, Li Z, Liu S, Zhang D. Global, regional and national burden of inflammatory bowel disease in 204 countries and territories from 1990 to 2019: a systematic analysis based on the global burden of disease study 2019. BMJ Open. (2023) 13:e065186. doi: 10.1136/bmjopen-2022-065186, PMID: - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources

