Impact of high-intensity interval training on cardiometabolic health in patients with diabesity: a systematic review and meta-analysis of randomized controlled trials
- PMID: 41137077
- PMCID: PMC12553184
- DOI: 10.1186/s13098-025-01974-4
Impact of high-intensity interval training on cardiometabolic health in patients with diabesity: a systematic review and meta-analysis of randomized controlled trials
Abstract
Aims: This systematic review and meta-analysis aimed to evaluate the effects of high-intensity interval training (HIIT) on cardiometabolic health-related outcomes in patients with type 2 diabetes and obesity (diabesity).
Methods: PubMed, Web of Science, Scopus, Science Direct, Cochrane Library, and Google Scholar databases were searched from inception up to November 2024. The search strategy encompassed the following keywords: diabetes, obesity, and HIIT. Randomized controlled trials (RCTs) recruiting adult participants with diabesity and comparing HIIT per se for ≥ 2 weeks in duration with non-exercise standard treatment were included.
Results: A total of 18 RCTs qualified involving 504 patients (52/48 women/men ratio; 55.0 ± 11.8 years; 31.0 ± 6.9 kg/m2). Body mass [standardized mean differences (SMD) -0.36 kg, 95% confidence intervals (CI) -0.71 to -0.01], body mass index (SMD -0.57 kg/m2, 95% CI -0.92 to -0.21), waist-to-hip ratio (SMD -1.68, 95% CI -2.50 to -0.86), fasting blood glucose (SMD -0.64 mmol/L, 95% CI -1.03 to -0.24), glycated hemoglobin (SMD -1.08%, 95% CI -1.68 to -0.47), fasting insulin (SMD -0.79 mIU/L, 95% CI -1.28 to -0.31), homeostatic model assessment for insulin resistance (SMD -0.95, 95% CI -1.43 to -0.47), low-density lipoprotein cholesterol (SMD -0.64 mg/dL, 95% CI -1.23 to -0.06), triglycerides (SMD -0.64 mg/dL, 95% CI -1.02 to -0.26), and total cholesterol (SMD -0.66 mg/dL, 95% CI -1.23 to -0.08) improved compared to standard treatment without exercise.
Conclusions: The present findings suggest that HIIT improves several markers of metabolic health and cardiovascular risk, even without significant body composition improvements in patients with diabesity. OPEN SCIENCE FRAMEWORK REGISTRY.: https://osf.io/rtb42.
Keywords: Aerobic capacity; Blood pressure; Body composition; Exercise; Glucose metabolism; Intermittent training; Lipid metabolism; Obesity; Type 2 diabetes.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: Not applicable. Provenance and peer review: Not commissioned; externally peer-reviewed. Patient consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures
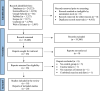


References
Publication types
LinkOut - more resources
Full Text Sources

