Predicting short- to long-term breast cancer risk from longitudinal mammographic screening history
- PMID: 41162416
- PMCID: PMC12572377
- DOI: 10.1038/s41523-025-00831-x
Predicting short- to long-term breast cancer risk from longitudinal mammographic screening history
Abstract
Breast cancer (BC) risk assessment aims to enhance individualized screening and prevention strategies. While recent deep learning (DL) models based on mammography have shown promise in short-term risk prediction, they primarily rely on single-time-point (STP) exams, ignoring temporal changes in breast tissue from sequence exams. We present the Multi-Time Point Breast Cancer Risk Model (MTP-BCR), a novel DL approach that integrates traditional risk factors and longitudinal mammography data to capture subtle tissue changes indicative of future malignancy. Using a large in-house dataset with 171,168 mammograms from 9133 women, MTP-BCR achieved superior performance in 10-year risk prediction, with an AUC of 0.80 (95% CI, 0.78-0.82) at the patient level, outperforming STP-based and traditional risk models. External validation on the CSAW-CC dataset confirmed its robustness. Further analysis demonstrates the advantages of the MTP-BCR method in diverse populations. MTP-BCR also excels in risk stratification and offers heatmaps to enhance clinical interpretability.
© 2025. The Author(s).
Conflict of interest statement
Competing interests: J.T., Associate editor for NPJ Breast Cancer. The remaining authors declare no competing interests.
Figures




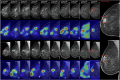
References
-
- Anderson, B. O. et al. The Global Breast Cancer Initiative: a strategic collaboration to strengthen health care for non-communicable diseases. Lancet Oncol.22, 578–581 (2021). - PubMed
-
- Pace, L. E. & Keating, N. L. A systematic assessment of benefits and risks to guide breast cancer screening decisions. JAMA311, 1327–1335 (2014). - PubMed
-
- McKinney, S. M. et al. International evaluation of an AI system for breast cancer screening. Nature577, 89–94 (2020). - PubMed
-
- Lauby-Secretan, B. et al. Breast-cancer screening—viewpoint of the IARC Working Group. N. Engl. J. Med.372, 2353–2358 (2015). - PubMed
LinkOut - more resources
Full Text Sources

