Longitudinal changes in hippocampal morphology before and after temporal lobe epilepsy surgery
- PMID: 41229613
- PMCID: PMC12603362
- DOI: 10.1093/braincomms/fcaf416
Longitudinal changes in hippocampal morphology before and after temporal lobe epilepsy surgery
Abstract
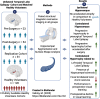
Temporal lobe epilepsy (TLE) is associated with progressive neocortical thinning that may be prevented by resective surgery, but little knowledge exists on dynamic changes in the hippocampus. Here, we assessed progressive morphological changes of the hippocampus before and after TLE surgery. In this longitudinal case-control neuroimaging study, we included patients with unilateral drug-resistant TLE before (main cohort n = 23; replication cohort n = 81) or after (n = 54) anterior temporal lobe resection and healthy volunteers (n = 120) matched for age and sex. We compared hippocampal volumes and surface shape morphology on paired scans between groups using linear mixed effects models. We did not find accelerated atrophy of the ipsilateral hippocampus in chronic presurgical TLE (-2.1 µl/year) compared to normal aging (-3.6 µl/year, P = 0.78). In contrast, there was progressive hypertrophy of the contralateral hippocampus before epilepsy surgery (+1.4 µl/year) compared to normal aging (-4.1 µl/year), which was further accelerated after surgery (+4.0 µl/year, P = 0.01). We validated these findings in the replication cohort (n = 81). Factors contributing to contralateral hippocampal hypertrophy included left-sided epilepsy lateralization, ipsilateral hippocampal sclerosis, and visual memory encoding deficits before or after surgery. Conversely, a history of focal to bilateral tonic clonic seizures was associated with accelerated pre- and postsurgical atrophy of the contralateral hippocampus. Refractory TLE is associated with progressive hypertrophy of the contralateral hippocampus before and after resective surgery. These contralateral changes may represent compensatory plasticity that is related to pre- and postoperative disturbances in cognition, mainly affecting visual memory. In contrast to progressive cortical thinning, the ipsilateral hippocampus does not show additional atrophy in chronic TLE.
Keywords: MRI; epilepsy; hippocampus; seizures; surgery.
© The Author(s) 2025. Published by Oxford University Press on behalf of the Guarantors of Brain.
Conflict of interest statement
Marian Galovic received fees and travel support from Advisis, Angelini, Bial, Eisai, and UCB outside the submitted work. Other authors do not report conflicts of interest.
Figures





References
-
- Engel J Jr. Introduction to temporal lobe epilepsy. Epilepsy Res. 1995;26(1):141–150.
-
- Margerison J, Corsellis J. Epilepsy and the temporal lobes: A clinical, electroencephalographic and neuropathological study of the brain in epilepsy, with particular reference to the temporal lobes. Brain. 1966;89(3):499–530. - PubMed
-
- Wieser H. Mesial temporal lobe epilepsy with hippocampal sclerosis. Epilepsia. 2004;45(6):695–714. - PubMed
LinkOut - more resources
Full Text Sources
