Association Between Health Insurance Type and Survival Outcomes: Insight Into the Impact of Socioeconomic Disparities in the Postoperative Outcomes of Abdominal Aortic Aneurysm in Korea
- PMID: 41287482
- PMCID: PMC12643959
- DOI: 10.3346/jkms.2025.40.e238
Association Between Health Insurance Type and Survival Outcomes: Insight Into the Impact of Socioeconomic Disparities in the Postoperative Outcomes of Abdominal Aortic Aneurysm in Korea
Abstract
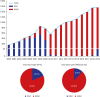
Background: Abdominal aortic aneurysm (AAA) is associated with a high mortality rate if left untreated, and medically vulnerable populations experience significant disparities in treatment and outcomes. We investigated the characteristics and treatment outcomes of AAA according to the insurance type (i.e., National Health Insurance [NHI] and Medical Aid) in South Korea using the nationwide health insurance database.
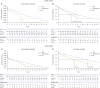
Methods: From 2002 to 2019, a total of 15,065 patients underwent either open aneurysm repair (OAR) or endovascular aneurysm repair (EVAR). The primary outcome was AAA-related mortality, with follow-up conducted until death or December 31, 2019, for those without mortality records. Mortality was evaluated using Kaplan-Meier curves and an adjusted Cox proportional hazards model to identify independent risk factors for AAA-related mortality. Propensity score matching (PSM) was employed using relevant covariates to achieve a 1:10 match between the NHI and Medical Aid groups.
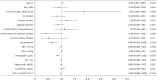
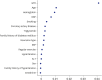
Results: Among the EVAR patients, the rate of AAA-related mortality was significantly higher in the Medical Aid group compared to the NHI group (P < 0.001). After adjusting for covariates, the difference in AAA-related mortality rates between the two insurance groups remained statistically significant. No significant difference was found between the two groups among OAR patients (P = 0.727). Factors such as age, insurance type, hypertension, diastolic blood pressure, hemoglobin levels, and glomerular filtration rate were significantly associated with AAA-related mortality in the unadjusted multivariable analysis among the EVAR patients. Specifically, Medical Aid patients had a 1.87-fold higher risk of AAA-related mortality compared to NHI patients. Notably, in the PSM cohort, multivariable analysis confirmed that insurance type remained a significant factor for AAA-related mortality in EVAR patients.
Conclusion: In patients undergoing EVAR for AAA, insurance type was independently associated with postoperative AAA-related mortality, with Medical Aid patients experiencing worse outcomes. In contrast, no significant difference in AAA-related mortality was observed between insurance types among patients undergoing OAR. These findings highlight the need to improve postoperative care and address outcome disparities in vulnerable populations undergoing EVAR.
Keywords: Abdominal Aortic Aneurysms; Endovascular Aneurysm Repair; Health Insurance; Healthcare Disparities; Mortality; Open Aneurysm Repair.
© 2025 The Korean Academy of Medical Sciences.
Conflict of interest statement
The authors have no potential conflicts of interest to disclose.
Figures


References
-
- Gao JP, Guo W. Mechanisms of abdominal aortic aneurysm progression: a review. Vasc Med. 2022;27(1):88–96. - PubMed
-
- Summers KL, Kerut EK, Sheahan CM, Sheahan MG., 3rd Evaluating the prevalence of abdominal aortic aneurysms in the United States through a national screening database. J Vasc Surg. 2021;73(1):61–68. - PubMed
-
- Eldrup-Jorgensen J, Kraiss LW, Chaikof EL, Neal D, Forbes TL. Vascular Quality Initiative assessment of compliance with Society for Vascular Surgery clinical practice guidelines on the care of patients with abdominal aortic aneurysm. J Vasc Surg. 2020;72(3):874–885. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

