Transplantation of congenitally opaque corneas
- PMID: 9497466
- PMCID: PMC1722090
- DOI: 10.1136/bjo.81.12.1064
Transplantation of congenitally opaque corneas
Abstract
Aims: To assess retrospectively the prognosis and complications of corneal grafting for congenital opacities.
Methods: Fifty eight eyes of infants and young children with congenital corneal opacities were studied retrospectively. Preoperative diagnoses included sclerocornea (27 eyes), Peters' anomaly (17 eyes), partial sclerocornea (12 eyes), and congenital glaucoma (two eyes). Penetrating keratoplasty was performed between 5 days and 65 months of age with a mean follow up of 40 (SD 29) months.
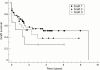
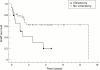
Results: The overall success (including regrafts) was 70% in eyes with sclerocornea, 83% for partial sclerocornea, and 100% for Peters' anomaly. However, 23 eyes had to be regrafted between 2 weeks and 110 months postoperatively. The probability of maintaining a clear graft, calculated by survival analysis, was 75% (SE 6%) at 1 year and 58% (7%) at 2 years for the entire group. Complications included cataract development (12 eyes), secondary glaucoma (14 eyes), epithelial defects (six eyes), band keratopathy (five eyes), retinal detachment (three eyes), wound leakage (two eyes), retrocorneal membrane (one eye), and microbial keratitis (two eyes).
Conclusions: It is concluded that corneal grafting for congenital opacities in infants has an excellent potential for long term survival and should be performed as early as possible for unilateral as well as bilateral involvement. The postoperative course is complex and often requires regrafting.
Figures

Similar articles
-
Long-term visual prognosis in children after corneal transplant surgery for Peters anomaly type I.Am J Ophthalmol. 2007 Jul;144(1):104-108. doi: 10.1016/j.ajo.2007.03.058. Am J Ophthalmol. 2007. PMID: 17601429
-
Surgical management of glaucoma in infants and children with Peters' anomaly: long-term structural and functional outcome.Ophthalmology. 2004 Jan;111(1):112-7. doi: 10.1016/j.ophtha.2003.02.002. Ophthalmology. 2004. PMID: 14711722
-
Long-term results of corneal graft survival in infants and children with peters anomaly.Ophthalmology. 1999 Apr;106(4):833-48. doi: 10.1016/S0161-6420(99)90175-6. Ophthalmology. 1999. PMID: 10201611
-
Peters' anomaly: a review of 26 penetrating keratoplasties in infants.Ophthalmic Surg. 1993 Jan;24(1):31-5. Ophthalmic Surg. 1993. PMID: 8446330 Review.
-
Peters Anomaly: Novel Non-Invasive Alternatives to Penetrating Keratoplasty.Semin Ophthalmol. 2023 Apr;38(3):275-282. doi: 10.1080/08820538.2023.2176238. Epub 2023 Feb 14. Semin Ophthalmol. 2023. PMID: 36788651 Review.
Cited by
-
Clinicopathological correlation of congenital corneal opacification using ultrasound biomicroscopy.Br J Ophthalmol. 2002 Jan;86(1):62-9. doi: 10.1136/bjo.86.1.62. Br J Ophthalmol. 2002. PMID: 11801506 Free PMC article.
-
Pediatric corneal transplantation: techniques, challenges, and outcomes.Ther Adv Ophthalmol. 2024 Mar 25;16:25158414241237906. doi: 10.1177/25158414241237906. eCollection 2024 Jan-Dec. Ther Adv Ophthalmol. 2024. PMID: 38533487 Free PMC article. Review.
-
[Diagnostics, clinical aspects and genetics of congenital corneal opacities].Ophthalmologe. 2022 May;119(5):443-452. doi: 10.1007/s00347-022-01587-6. Epub 2022 Mar 4. Ophthalmologe. 2022. PMID: 35244750 Review. German.
-
Overview of sclerocornea.Taiwan J Ophthalmol. 2023 Nov 23;13(4):461-466. doi: 10.4103/tjo.TJO-D-23-00070. eCollection 2023 Oct-Dec. Taiwan J Ophthalmol. 2023. PMID: 38249514 Free PMC article. Review.
-
The Palisades of Vogt in Congenital Corneal Opacification (An American Ophthalmological Society Thesis).Trans Am Ophthalmol Soc. 2016 Aug;114:T8. Trans Am Ophthalmol Soc. 2016. PMID: 28042184 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
