Mechanism of injury-provoked poliomyelitis
- PMID: 9573275
- PMCID: PMC110068
- DOI: 10.1128/JVI.72.6.5056-5060.1998
Mechanism of injury-provoked poliomyelitis
Abstract
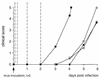
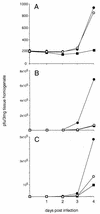
Skeletal muscle injury is known to predispose its sufferers to neurological complications of concurrent poliovirus infections. This phenomenon, labeled "provocation poliomyelitis," continues to cause numerous cases of childhood paralysis due to the administration of unnecessary injections to children in areas where poliovirus is endemic. Recently, it has been reported that intramuscular injections may also increase the likelihood of vaccine-associated paralytic poliomyelitis in recipients of live attenuated poliovirus vaccines. We have studied this important risk factor for paralytic polio in an animal system for poliomyelitis and have determined the pathogenic mechanism linking intramuscular injections and provocation poliomyelitis. Skeletal muscle injury induces retrograde axonal transport of poliovirus and thereby facilitates viral invasion of the central nervous system and the progression of spinal cord damage. The pathogenic mechanism of provocation poliomyelitis may differ from that of polio acquired in the absence of predisposing factors.
Figures


Similar articles
-
Intramuscular injections within 30 days of immunization with oral poliovirus vaccine--a risk factor for vaccine-associated paralytic poliomyelitis.N Engl J Med. 1995 Feb 23;332(8):500-6. doi: 10.1056/NEJM199502233320804. N Engl J Med. 1995. PMID: 7830731
-
Limited trafficking of a neurotropic virus through inefficient retrograde axonal transport and the type I interferon response.PLoS Pathog. 2010 Mar 5;6(3):e1000791. doi: 10.1371/journal.ppat.1000791. PLoS Pathog. 2010. PMID: 20221252 Free PMC article.
-
Random selection: a model for poliovirus infection of the central nervous system.J Gen Virol. 1997 Aug;78 ( Pt 8):1819-28. doi: 10.1099/0022-1317-78-8-1819. J Gen Virol. 1997. PMID: 9266975
-
Poliovirus biology and pathogenesis.Curr Top Microbiol Immunol. 1996;206:305-25. doi: 10.1007/978-3-642-85208-4_15. Curr Top Microbiol Immunol. 1996. PMID: 8608722 Review. No abstract available.
-
One hundred years of poliovirus pathogenesis.Virology. 2006 Jan 5;344(1):9-16. doi: 10.1016/j.virol.2005.09.015. Virology. 2006. PMID: 16364730 Review.
Cited by
-
Epidemics to eradication: the modern history of poliomyelitis.Virol J. 2007 Jul 10;4:70. doi: 10.1186/1743-422X-4-70. Virol J. 2007. PMID: 17623069 Free PMC article. Review.
-
Poly(rC) binding proteins mediate poliovirus mRNA stability.RNA. 2001 Aug;7(8):1126-41. doi: 10.1017/s1355838201010044. RNA. 2001. PMID: 11497431 Free PMC article.
-
Receptor (CD155)-dependent endocytosis of poliovirus and retrograde axonal transport of the endosome.J Virol. 2004 Jul;78(13):7186-98. doi: 10.1128/JVI.78.13.7186-7198.2004. J Virol. 2004. PMID: 15194795 Free PMC article.
-
Human tryptophanyl-tRNA synthetase is an IFN-γ-inducible entry factor for Enterovirus.J Clin Invest. 2018 Nov 1;128(11):5163-5177. doi: 10.1172/JCI99411. Epub 2018 Oct 15. J Clin Invest. 2018. PMID: 30153112 Free PMC article.
-
Receptor-dependent and -independent axonal retrograde transport of poliovirus in motor neurons.J Virol. 2009 May;83(10):4995-5004. doi: 10.1128/JVI.02225-08. Epub 2009 Feb 25. J Virol. 2009. PMID: 19244317 Free PMC article.
References
-
- Anderson G, Skaar A. Poliomyelitis occurring after antigen injections. Pediatrics. 1962;7:741–759. - PubMed
-
- Bodian D. Viremia, invasiveness, and the influence of injections. Ann NY Acad Sci. 1955;61:877–882. - PubMed
-
- Bodian D. Viremia in experimental poliomyelitis. II. Viremia and the mechanism of the “provoking effect” of injections or trauma. Am J Hyg. 1954;60:358–370. - PubMed
-
- Curtis R, Adryan K M, Zhu Y, Harkness P J, Lindsay R M, DiStefano P S. Retrograde axonal transport of ciliary neurotrophic factor is increased by peripheral nerve injury. Nature. 1993;365:253–255. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

