Pseudomonas aeruginosa exoenzyme S is a mitogen but not a superantigen for human T lymphocytes
- PMID: 9632568
- PMCID: PMC108315
- DOI: 10.1128/IAI.66.7.3072-3079.1998
Pseudomonas aeruginosa exoenzyme S is a mitogen but not a superantigen for human T lymphocytes
Abstract
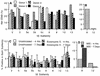
Virtually all cystic fibrosis (CF) patients become infected with Pseudomonas aeruginosa, and once the infection is established, the organism is rarely cleared. One of the P. aeruginosa virulence factors, exoenzyme S, has been shown to correlate with increased morbidity and mortality both in rat models of chronic pulmonary inflammation and in human CF patients. It has previously been shown that exoenzyme S is a potent stimulus for the proliferation of T cells in greater than 95% of adults, which could contribute to the pathogenesis of CF. The goal of this study was to determine the mechanism of T-cell stimulation by exoenzyme S in an effort to shed light on the immune response and contribute to understanding its role in P. aeruginosa pathogenesis. The current studies demonstrate that exoenzyme S stimulates naive T cells, since fetal blood lymphocytes proliferated and adult lymphocytes that expressed CD45RA proliferated. The percentage of T cells activated by exoenzyme S after a 4-h culture (as measured by CD69 surface expression) was intermediate in magnitude compared to levels induced by a panel of superantigens and mitogens. To determine the mechanism of activation, the requirement for accessory cells was investigated. The proliferative response to exoenzyme S was dependent on the presence of accessory cells but was not blocked by an anti-DR antibody. Exoenzyme S activated both CD4(+) and CD8(+) T cells, but CD4(+) T cells were preferentially activated. The Vbeta repertoire of donor T cells showed no preferential activation or preferential expansion after stimulation by exoenzyme S, suggesting that it is not a superantigen. Taken together, our data suggest that exoenzyme S is a T-cell mitogen but not a superantigen. Activation of a large percentage of T lymphocytes by exoenzyme S may produce a lymphocyte-mediated inflammatory response that should be considered in the pathogenesis of CF.
Figures


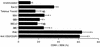



Similar articles
-
Pseudomonas aeruginosa exoenzyme S stimulates murine lymphocyte proliferation in vitro.Infect Immun. 1999 Sep;67(9):4613-9. doi: 10.1128/IAI.67.9.4613-4619.1999. Infect Immun. 1999. PMID: 10456907 Free PMC article.
-
Pseudomonas aeruginosa exoenzyme S induces proliferation of human T lymphocytes.Infect Immun. 1995 May;63(5):1800-5. doi: 10.1128/iai.63.5.1800-1805.1995. Infect Immun. 1995. PMID: 7537248 Free PMC article.
-
Exoenzyme S from Pseudomonas aeruginosa induces apoptosis in T lymphocytes.J Leukoc Biol. 2000 Jun;67(6):808-16. doi: 10.1002/jlb.67.6.808. J Leukoc Biol. 2000. PMID: 10857853
-
Genetic analysis of exoenzyme S expression by Pseudomonas aeruginosa.FEMS Microbiol Lett. 1996 Jan 15;135(2-3):149-55. doi: 10.1111/j.1574-6968.1996.tb07981.x. FEMS Microbiol Lett. 1996. PMID: 8595851 Review.
-
The exoenzyme S regulon of Pseudomonas aeruginosa.Mol Microbiol. 1997 Nov;26(4):621-9. doi: 10.1046/j.1365-2958.1997.6251991.x. Mol Microbiol. 1997. PMID: 9427393 Review.
Cited by
-
State of the art: why do the lungs of patients with cystic fibrosis become infected and why can't they clear the infection?Respir Res. 2003;4(1):8. doi: 10.1186/1465-9921-4-8. Epub 2003 Aug 27. Respir Res. 2003. PMID: 14511398 Free PMC article. Review.
-
Pseudomonas aeruginosa exoenzyme S induces transcriptional expression of proinflammatory cytokines and chemokines.Infect Immun. 2000 Aug;68(8):4811-4. doi: 10.1128/IAI.68.8.4811-4814.2000. Infect Immun. 2000. PMID: 10899895 Free PMC article.
-
Pseudomonas aeruginosa exoenzyme S stimulates murine lymphocyte proliferation in vitro.Infect Immun. 1999 Sep;67(9):4613-9. doi: 10.1128/IAI.67.9.4613-4619.1999. Infect Immun. 1999. PMID: 10456907 Free PMC article.
-
Abnormal functional lymphoid tolerance and enhanced myeloid exocytosis are characteristics of resting and stimulated PBMCs in cystic fibrosis patients.Front Immunol. 2024 Feb 26;15:1360716. doi: 10.3389/fimmu.2024.1360716. eCollection 2024. Front Immunol. 2024. PMID: 38469306 Free PMC article.
References
-
- Abe J, Forrester J, Nakahara T, Lafferty J A, Kotzin B L, Leung D Y. Selective stimulation of human T cells with streptococcal erythrogenic toxins A and B. J Immunol. 1991;146:3747–3750. - PubMed
-
- Andersson J, Nagy S, Bjork L, Abrams J, Holm S, Andersson U. Bacterial toxin-induced cytokine production studied at the single-cell level. Immunol Rev. 1992;127:69–96. - PubMed
-
- Azzawi M, Johnston P W, Majumdar S, Kay A B, Jeffrey P K. T lymphocytes and activated eosinophils in airway mucosa in fatal asthma and cystic fibrosis. Am Rev Respir Dis. 1992;145:1477–1482. - PubMed
-
- Bacon K B, Premack B A, Gardner P, Schall T J. Activation of dual T cell signalling pathways by the chemokine RANTES. Science. 1995;269:1727–1730. - PubMed
-
- Biselli R, Matricardi P M, D’Amelio R, Fattorossi A. Multiparametric flow cytometric analysis of the kinetics of surface molecule expression after polyclonal activation of human peripheral blood T lymphocytes. Scand J Immunol. 1992;35:439–447. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials

