Compartmentalized transgene expression of granulocyte-macrophage colony-stimulating factor (GM-CSF) in mouse lung enhances allergic airways inflammation
- PMID: 9717963
- PMCID: PMC1905049
- DOI: 10.1046/j.1365-2249.1998.00652.x
Compartmentalized transgene expression of granulocyte-macrophage colony-stimulating factor (GM-CSF) in mouse lung enhances allergic airways inflammation
Abstract
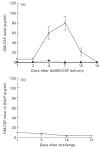
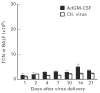
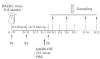
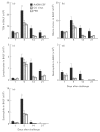
To investigate the role of GM-CSF in asthmatic airways inflammation, we have targeted GM-CSF transgene to the airway cells in a mouse model of ovalbumin (OVA)-induced allergic airways inflammation, a model in which there is marked induction of endogenous IL-5 and IL-4 but not GM-CSF. Following intranasal delivery of a replication-deficient adenoviral gene transfer vector (Ad), transgene expression was found localized primarily to the respiratory epithelial cells. Intranasal delivery of 0.03 x 10(9) plaque-forming units (PFU) of AdGM-CSF into naive BALB/c mice resulted in prolonged and compartmentalized release of GM-CSF transgene protein with a peak concentration of approximately 80 pg/ml detected in bronchoalveolar lavage fluid (BALF) at day 7, but little in serum. These levels of local GM-CSF expression per se resulted in no eosinophilia and only a minimum of tissue inflammatory responses in the lung of naive mice, similar to those induced by the control vector. However, such GM-CSF expression in the airways of OVA-sensitized mice resulted in a much greater and sustained accumulation of various inflammatory cell types, most noticeably eosinophils, both in BALF and airway tissues for 15-21 days post-OVA aerosol challenge, at which times airways inflammation had largely resolved in control mice. While the levels of IL-5 and IL-4 in BALF and the rate of eosinophil apoptosis were found similar between different treatments, there was an increased number of proliferative leucocytes in the lung receiving GM-CSF gene transfer. Our results thus provide direct experimental evidence that GM-CSF can significantly contribute to the development of allergic airways inflammation through potentiating and prolonging inflammatory infiltration induced by cytokines such as IL-5 and IL-4.
Figures
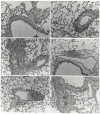
References
-
- Bochner BS, Undem BJ, Lichtenstein LM. Immunological aspects of allergic asthma. Ann Rev Immunol. 1994;12:295–335. - PubMed
-
- Bousquet J, Chanez P, Vignola AM, Lacoste J-V, Michel FB. Eosinophil inflammation in asthma. Am J Respir Crit Care Med. 1994;150:S33–S38. - PubMed
-
- Walker C, Kaegi MK, Braun P, Blaser K. Activated T cells and eosinophilia in bronchoalveolar lavages from subjects with asthma correlated with disease severity. J Allergy Clin Immunol. 1991;88:935–42. - PubMed
-
- Weller PF. The immunobiology of eosinophils. N Engl J Med. 1991;324:1110–8. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

