Complement activation in relation to capillary leakage in children with septic shock and purpura
- PMID: 9784543
- PMCID: PMC108669
- DOI: 10.1128/IAI.66.11.5350-5356.1998
Complement activation in relation to capillary leakage in children with septic shock and purpura
Abstract
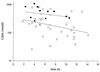
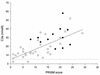
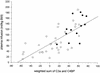
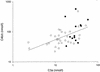
To assess the relationship between capillary leakage and inflammatory mediators during sepsis, blood samples were taken on hospital admission, as well as 24 and 72 h later, from 52 children (median age, 3.3 years) with severe meningococcal sepsis, of whom 38 survived and 14 died. Parameters related to cytokines (interleukin 6 [IL-6] IL-8, plasma phospholipase A2, and C-reactive protein [CRP]), to neutrophil degranulation (elastase and lactoferrin), to complement activation (C3a, C3b/c, C4b/c, and C3- and C4-CRP complexes), and to complement regulation (functional and inactivated C1 inhibitor and C4BP) were determined. The degree of capillary leakage was derived from the amount of plasma infused and the severity of disease by assessing the pediatric risk of mortality (PRISM) score. Levels of IL-6, IL-8, C3b/c, C3-CRP complexes, and C4BP on admission, adjusted for the duration of skin lesions, were significantly different in survivors and nonsurvivors (C3b/c levels were on average 2.2 times higher in nonsurvivors, and C3-CRP levels were 1.9 times higher in survivors). Mortality was independently related to the levels of C3b/c and C3-CRP complexes. In agreement with this, levels of complement activation products correlated well with the PRISM score or capillary leakage. Thus, these data show that complement activation in patients with severe meningococcal sepsis is associated with a poor outcome and a more severe disease course. Further studies should reveal whether complement activation may be a target for therapeutical intervention in this disease.
Figures


References
-
- Bone R C. Inhibitors of complement and neutrophils: a critical evaluation of their role in the treatment of sepsis. Crit Care Med. 1992;20:891–898. - PubMed
-
- Brandtzaeg P. Systemic meningococcal disease: clinical pictures and pathophysiological background. Rev Med Microbiol. 1996;7:63–72.
-
- Brandtzaeg P, Hogasen K, Kierulf P, Mollnes T E. The excessive complement activation in fulminant meningococcal septicemia is predominantly caused by alternative pathway activation. J Infect Dis. 1996;173:647–655. - PubMed
-
- Brandtzaeg P B, Mollnes T E, Kierulf P. Complement activation and endotoxin levels in systemic meningococcal disease. J Infect Dis. 1989;160:58–65. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

