Primary drug resistance in South Africa: data from 10 years of surveys
- PMID: 22251009
- PMCID: PMC3358100
- DOI: 10.1089/aid.2011.0284
Primary drug resistance in South Africa: data from 10 years of surveys
Abstract
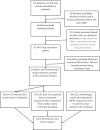
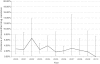
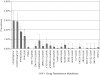
HIV-1 transmitted drug resistance (TDR) could reverse the gains of antiretroviral rollout. To ensure that current first-line therapies remain effective, TDR levels in recently infected treatment-naive patients need to be monitored. A literature review and data mining exercise was carried out to determine the temporal trends in TDR in South Africa. In addition, 72 sequences from seroconvertors identified from Africa Centre's 2010 HIV surveillance round were also examined for TDR. Publicly available data on TDR were retrieved from GenBank, curated in RegaDB, and analyzed using the Calibrated Population Resistance Program. There was no evidence of TDR from the 2010 rural KwaZulu Natal samples. Ten datasets with a total of 1618 sequences collected between 2000 and 2010 were pooled to provide a temporal analysis of TDR. The year with the highest TDR rate was 2002 [6.67%, 95% confidence interval (CI): 3.09-13.79%; n=6/90]. After 2002, TDR levels returned to <5% (WHO low-level threshold) and showed no statistically significant increase in the interval between 2002 and 2010. The most common mutations were associated with NNRTI resistance, K103N, followed by Y181C and Y188C/L. Five sequences had multiple resistance mutations associated with NNRTI resistance. There is no evidence of TDR in rural KwaZulu-Natal. TDR levels in South Africa have remained low following a downward trend since 2003. Continuous vigilance in monitoring of TDR is needed as more patients are initiated and maintained onto antiretroviral therapy.
Figures
References
-
- Popp D. Fisher JD. First, do no harm: A call for emphasizing adherence and HIV prevention interventions in active antiretroviral therapy programs in the developing world. AIDS. 2002;16(4):676–678. - PubMed
-
- Trotta MP. Ammassari A. Melzi S, et al. Treatment-related factors and highly active antiretroviral therapy adherence. J Acquir Immune Defic Syndr. 2002;31(Suppl 3):S128–131. - PubMed
-
- Uzochukwu BS. Onwujekwe OE. Onoka AC. Okoli C. Uguru NP. Chukwuogo OI. Determinants of non-adherence to subsidized anti-retroviral treatment in southeast Nigeria. Health Policy Plan. 2009;24(3):189–196. - PubMed
-
- Mills EJ. Nachega JB. Buchan I, et al. Adherence to antiretroviral therapy in sub-Saharan Africa and North America: A meta-analysis. JAMA. 2006;296(6):679–690. - PubMed
Publication types
MeSH terms
Substances
Associated data
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
- Actions
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases